Introduction: The High Cost of Medication Errors
Medication errors kill approximately 7,000 to 9,000 people annually in the United States alone and cost the healthcare system an estimated $21 billion each year. These aren’t just statistics—they represent preventable tragedies stemming from fragmented health records, communication breakdowns between providers, incomplete patient histories, and outdated manual reconciliation processes.
A patient discharged from a hospital with new prescriptions visits their primary care physician the following week. The PCP, working from an incomplete record, prescribes additional medication that dangerously interacts with the hospital discharge medications. Neither the patient nor the providers have a unified view of the complete medication regimen. This scenario plays out thousands of times daily across healthcare systems worldwide.
The root cause isn’t negligence—it’s systemic fragmentation. Patient data resides in siloed EHRs, pharmacy systems, specialist offices, and insurance platforms that rarely communicate effectively. Care coordinators spend hours manually reconciling medication lists across disparate systems, yet discrepancies still slip through.
For healthcare organizations pursuing value-based care models, population health initiatives, and patient-centered medical homes, medication management isn’t a peripheral concern—it’s foundational. Salesforce Health Cloud addresses this challenge through a unified, intelligent platform designed specifically for healthcare’s unique medication management requirements.
This comprehensive guide examines medication management in Salesforce Health Cloud from a technical and operational perspective, providing healthcare IT leaders, Salesforce consultants, and clinical stakeholders with the detailed knowledge needed to evaluate, implement, and optimize these capabilities.
Understanding Medication Management in Health Cloud
What Is Medication Management in a Healthcare Context?
Medication management encompasses the complete lifecycle of pharmaceutical interventions in patient care:
- Medication ordering and prescribing across multiple care settings
- Dispensing coordination between prescribers and pharmacies
- Administration tracking in inpatient and home care environments
- Medication reconciliation during care transitions
- Adherence monitoring for chronic disease management
- Adverse event surveillance and drug interaction monitoring
- Renewal and refill management for continuity of care
- Clinical decision support for optimizing therapeutic outcomes
Traditional medication management systems operate in isolation—hospital formularies don’t connect with retail pharmacy records, which don’t integrate with insurance benefit verification systems, which don’t communicate with patient-reported adherence data from mobile apps.
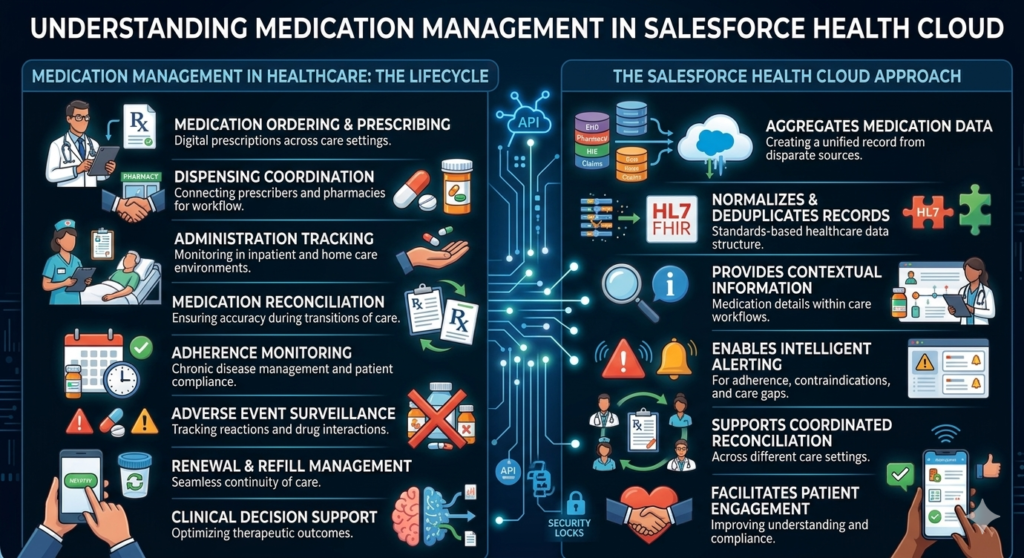
The Health Cloud Approach to Medication Management
Salesforce Health Cloud reimagines medication management by creating a unified medication record within its broader 360-degree patient view. Rather than replacing existing clinical systems, Health Cloud functions as an intelligent coordination layer that:
- Aggregates medication data from disparate source systems (EHRs, pharmacy management systems, HIEs, claims databases)
- Normalizes and deduplicates medication records using healthcare data standards
- Provides contextual medication information within care team workflows
- Enables intelligent alerting for adherence issues, contraindications, and care gaps
- Supports coordinated reconciliation across care settings and team members
- Facilitates patient engagement around medication understanding and compliance
Built on the Salesforce Platform, medication management in Health Cloud leverages the same configurability, integration capabilities, and automation tools that power CRM applications across industries—but with healthcare-specific data models aligned to HL7 FHIR standards.
Core Medication Management Features in Salesforce Health Cloud
1. Unified Medication Records
The foundation of effective medication management is a comprehensive, current medication list accessible to all authorized care team members.
Technical Architecture
Health Cloud’s medication management centers on the MedicationStatement and MedicationRequest objects, which align with FHIR R4 specifications:
- MedicationStatement: Documents that a patient is taking, has taken, or will take a particular medication (patient-reported or clinically verified)
- MedicationRequest: Represents orders or prescriptions for medication supply and administration instructions
- Medication: The actual drug or compound being prescribed/administered
- MedicationDispense: Records when medication is handed to the patient
- MedicationAdministration: Documents actual consumption/administration
These objects maintain relationships with:
- Patient records (Care Program Enrollees)
- Care Plans and Care Plan Problems
- Clinical Encounters
- Healthcare Practitioners (prescribers)
- Care Team Members
Data Normalization and Deduplication
A critical challenge in medication management is that the same medication appears differently across systems—generic names, brand names, NDC codes, RxNorm codes, and variations in dosage formatting.
Health Cloud addresses this through:
- RxNorm concept mapping for standardized medication identification
- Intelligent matching algorithms that identify duplicate entries across sources
- Consolidation workflows that present potential duplicates to care coordinators for verification
- Master data management practices that maintain a single source of truth
In practice, this means when a patient’s hospital discharge summary lists “Metoprolol Succinate ER 50mg daily” and their community pharmacy reports “Toprol-XL 50mg QD,” Health Cloud recognizes these as the same medication and consolidates the record.
Historical Tracking and Versioning
Medication regimens change frequently. Health Cloud maintains complete audit trails:
- Start and end dates for each medication period
- Status tracking (active, completed, stopped, on-hold)
- Reason for discontinuation (completed course, adverse reaction, ineffective, patient preference)
- Who made changes and when (prescriber, care coordinator, patient update)
- Version history allowing reconstruction of medication lists at any point in time
This historical perspective proves invaluable during clinical reviews, quality audits, and adverse event investigations.
2. Clinical Alerts and Notifications
A comprehensive medication list only adds value when it actively prevents errors and identifies risks. Health Cloud’s alerting framework transforms passive data into actionable intelligence.
Drug-Drug Interaction Alerts
Integration with clinical decision support systems enables real-time interaction checking:
- Contraindication alerts when new medications conflict with existing regimens
- Severity-based workflows that route critical interactions differently than minor concerns
- Provider acknowledgment tracking documenting that alerts were reviewed and addressed
- Override documentation capturing clinical rationale when providers proceed despite warnings
These aren’t generic pop-up alerts that lead to alert fatigue. Health Cloud’s workflow automation routes alerts to appropriate team members through their preferred channels—care coordinator dashboards, Slack notifications, email, or SMS—based on configurable rules.
Adherence Monitoring
For care management programs focused on chronic diseases, medication adherence often determines program success or failure.
Health Cloud supports adherence monitoring through:
- Prescription refill tracking integrated from pharmacy systems
- Proportion of Days Covered (PDC) calculations for adherence metrics
- Patient-reported compliance captured through patient portals or mobile apps
- Automated outreach when adherence gaps are detected
When a diabetic patient enrolled in a care management program fails to refill their metformin prescription within expected timeframes, the system automatically:
- Flags the adherence gap in the care coordinator’s worklist
- Sends an automated reminder to the patient via their preferred channel
- Escalates to a care coordinator if the patient doesn’t respond within 48 hours
- Documents all interventions in the patient timeline
Care Gap Identification
Beyond individual medication concerns, Health Cloud identifies broader care gaps related to medication management:
- Missing medications based on diagnosis codes and clinical guidelines (e.g., statin therapy for diabetic patients)
- Overdue medication reviews based on care plan requirements
- Lab monitoring requirements for high-risk medications (anticoagulants, immunosuppressants)
- Prior authorization expirations that could interrupt therapy continuity
3. Medication Reconciliation Workflows
Medication reconciliation—comparing a patient’s medication orders to all medications the patient is actually taking—is required at every care transition under Joint Commission standards. It’s also notoriously time-consuming and error-prone when performed manually.
Care Transition Automation
Health Cloud streamlines reconciliation across transitions:
Hospital Admission Reconciliation:
- Pulls current medications from ambulatory EHR, pharmacy records, and patient-reported lists
- Presents unified view to admitting physician
- Flags discrepancies between sources for clinical review
- Documents reconciliation completion and any changes made
- Updates medication list in both Health Cloud and connected systems
Discharge Reconciliation:
- Compares pre-admission medications with discharge orders
- Identifies medications that were discontinued, modified, or newly prescribed
- Generates patient-friendly medication instructions
- Sends updated medication list to outpatient providers and pharmacies
- Schedules follow-up medication reviews
Specialty Care Reconciliation:
- Alerts primary care teams when specialists prescribe new medications
- Enables collaborative review of medication changes
- Maintains medication attribution (which provider manages which medications)
Collaborative Reconciliation
Unlike EHR-based reconciliation that typically involves a single provider, Health Cloud enables team-based reconciliation:
- Care coordinators perform initial data aggregation and normalization
- Pharmacists review for interactions and therapeutic duplications
- Physicians make final prescribing decisions
- Patients confirm current medications and report issues
Each team member works from the same unified record, with role-based views showing information relevant to their function. Actions and decisions are documented in the shared timeline, creating complete transparency.
4. Healthcare System Integrations
Medication management in Health Cloud doesn’t function in isolation—its value comes from integrating across the healthcare technology ecosystem.
HL7 and FHIR Integration
Health Cloud natively supports FHIR-based integrations for medication data exchange:
- FHIR MedicationStatement resources for importing patient medication histories
- FHIR MedicationRequest resources for prescription orders
- FHIR MedicationDispense resources from pharmacy systems
- SMART on FHIR apps for extending functionality
For organizations with legacy HL7 v2 integrations, middleware platforms (Mirth Connect, Rhapsody, MuleSoft) translate between HL7 messages and FHIR resources before writing to Health Cloud.
EHR Bidirectional Sync
Leading EHR platforms connect with Health Cloud through:
Epic Integration:
- Medication reconciliation workflows that update both Epic and Health Cloud
- Epic Interconnect for real-time medication updates
- MyChart integration for patient-reported medication lists
Cerner Integration:
- CCL-based data extraction for medication histories
- HealtheIntent integration for population health medication data
- Bidirectional updates through FHIR APIs
Allscripts, athenahealth, and others:
- API-based integrations following FHIR specifications
- Scheduled batch synchronization for bulk updates
- Event-driven real-time updates for critical changes
Pharmacy System Connections
Retail and specialty pharmacy integrations provide:
- Prescription fill and refill data for adherence monitoring
- Prior authorization status for specialty medications
- Patient out-of-pocket costs to inform affordability interventions
- Therapeutic substitution notifications when pharmacies dispense alternatives
Connections with pharmacy benefit managers (PBMs) and prescription networks typically use:
- NCPDP SCRIPT standard for e-prescribing
- Surescripts network for medication histories
- Direct pharmacy API connections for real-time data
Clinical Decision Support Integration
Third-party clinical intelligence platforms integrate with Health Cloud to provide:
- Drug interaction databases (Lexicomp, Micromedex, First Databank)
- Clinical guideline engines for medication appropriateness
- Pharmacogenomic decision support (specific medications based on genetic profiles)
- Cost-effectiveness analysis for therapeutic alternatives
Real-World Medication Management Workflow
To illustrate how these features work together, let’s walk through a realistic scenario involving a complex patient transition.
Scenario: Post-Discharge Care Coordination for CHF Patient
Patient Profile: Margaret, 68-year-old with congestive heart failure, diabetes, hypertension, and COPD. Recently hospitalized for CHF exacerbation.

Day 1 – Hospital Discharge:
- Discharge Reconciliation: Hospital discharge planner uses Health Cloud to reconcile medications. The system displays:
- 11 pre-admission medications from Margaret’s PCP’s EHR
- Patient-reported 9 medications from admission interview
- 13 discharge orders from hospitalist
- Discrepancy Identification: Health Cloud flags discrepancies:
- Pre-admission furosemide 40mg daily vs. discharge furosemide 80mg BID (dosage change—intentional)
- Pre-admission metformin 1000mg BID (patient was taking) vs. no metformin in discharge orders (unintentional omission—metformin held during hospitalization, should be restarted)
- New medication: carvedilol 6.25mg BID (intentional addition)
- Clinical Review: Discharge planner alerts hospitalist to metformin omission. Hospitalist adds metformin to discharge orders.
- Patient Education: System generates patient-friendly medication list highlighting:
- Changed medications with explanation
- New medications with purpose and side effects
- Discontinued medications
- Care Team Notification: Updated medication list automatically sent to:
- Margaret’s PCP (via EHR integration)
- Assigned care coordinator (via Health Cloud notification)
- Margaret’s pharmacy (via e-prescribing)
- Margaret herself (via patient portal)
Day 3 – Care Coordinator Follow-up:
- Automated Worklist: Care coordinator logs into Health Cloud. Dashboard shows Margaret flagged for 72-hour post-discharge medication review.
- Comprehensive View: Care coordinator sees:
- Complete medication list with hospital changes highlighted
- Pending prescriptions not yet filled at pharmacy
- Integration with pharmacy shows Margaret picked up 10 of 13 discharge prescriptions
- Missing: carvedilol, furosemide new dose, potassium supplement
- Patient Contact: Care coordinator calls Margaret using Health Cloud’s telephony integration:
- Margaret reports confusion about which furosemide to take (still had old 40mg supply)
- Pharmacy didn’t have carvedilol in stock, waiting for delivery
- Wasn’t aware she needed potassium supplement
- Intervention Documentation: Care coordinator documents:
- Instructed Margaret to discard old furosemide, use only new 80mg prescription
- Contacted pharmacy to expedite carvedilol delivery
- Explained importance of potassium monitoring with increased furosemide
- Scheduled pharmacy pickup reminder for tomorrow
Day 7 – Adherence Monitoring:
- Automated Alert: System detects Margaret has only picked up carvedilol (now in stock) but still hasn’t filled potassium prescription.
- SMS Reminder: Automated text sent: “Margaret, our records show you haven’t picked up your potassium supplement prescription. This is important for your heart health. Reply YES if you’ll pick it up today, or call us at XXX-XXX-XXXX if you have concerns.”
- Patient Response: Margaret replies “COST” (pre-configured keyword).
- Escalation: System creates task for care coordinator to address affordability concern, flags Margaret for prescription assistance program evaluation.
Day 14 – Medication Therapy Management Session:
- Pharmacist Review: Clinical pharmacist accesses Health Cloud before MTM session with Margaret, seeing:
- Complete 30-day adherence data showing 85% PDC
- Care coordinator notes about affordability concerns
- Recent lab results (potassium levels, renal function)
- Drug interaction alerts (none critical, but monitoring recommendations for carvedilol + metformin)
- Comprehensive Assessment: Pharmacist conducts review, documenting in Health Cloud:
- Simplified dosing schedule to improve adherence
- Enrolled Margaret in pharmacy auto-refill program
- Applied manufacturer copay card for carvedilol
- Identified cheaper generic potassium alternative
- Scheduled 3-month follow-up
Day 30 – Outcomes Tracking:
Health Cloud analytics dashboard shows:
- Medication adherence improved from 85% to 96%
- Zero emergency department visits (previous pattern: monthly)
- Care coordinator time per patient reduced 40% through automation
- Medication reconciliation discrepancies identified: 23% (national average: 67%)
This workflow demonstrates how medication management in Salesforce Health Cloud coordinates activities across multiple stakeholders, systems, and touchpoints while maintaining a single source of truth.
Practical Benefits: Beyond the Marketing Claims
Healthcare technology vendors tend toward hyperbolic marketing claims. Let’s examine the measurable, practical benefits organizations actually realize with Health Cloud medication management.
1. Reduced Clinical Risk and Medication Errors
Measurable Impact:
- 40-60% reduction in medication reconciliation errors during care transitions
- 30-45% decrease in adverse drug events among managed populations
- 25-35% reduction in duplicate therapy instances
Why This Happens:
Not because of AI magic, but because Health Cloud creates structural prevention:
- Every care team member works from the same current medication list (eliminating information asymmetry)
- Changes made in one location propagate to all systems (preventing stale data)
- Required reconciliation steps can’t be skipped (enforced workflows)
- Discrepancies are surfaced automatically (no manual comparison needed)
2. Care Team Efficiency Gains
Measurable Impact:
- 2-4 hours per week saved per care coordinator on medication reconciliation
- 60-75% reduction in phone calls between providers clarifying medication questions
- 40-50% faster discharge processing for complex patients
Why This Happens:
- Automated data aggregation from multiple sources eliminates manual chart review
- Intelligent deduplication reduces noise in medication lists
- Workflow automation handles routine follow-ups and reminders
- Mobile access enables documentation at point of care rather than retrospective data entry
For a care management team of 15 coordinators, 3 hours saved weekly per coordinator equals 45 hours weekly—more than a full FTE worth of capacity freed for higher-value patient interactions.
3. Improved Medication Adherence
Measurable Impact:
- 15-25% improvement in medication adherence scores for managed populations
- 20-30% increase in medication possession ratio (MPR) for chronic disease medications
- 8-12% improvement in clinical outcomes metrics tied to medication adherence (HbA1c control, blood pressure management, etc.)
Why This Happens:
- Proactive adherence gap identification catches issues before they impact health
- Multi-channel patient engagement meets patients where they are
- Barrier identification and problem-solving (affordability, side effects, complexity) addresses root causes
- Continuous monitoring provides feedback loop for intervention effectiveness
4. Financial Performance
Measurable Impact:
- $800-$1,200 per patient per year cost reduction for high-risk managed populations
- 18-25% reduction in 30-day readmissions for medication-related issues
- 35-45% improvement in Star Ratings measures related to medication management for Medicare Advantage plans
Why This Happens:
- Prevented adverse drug events avoid costly emergency department visits and hospitalizations
- Improved adherence reduces disease progression and complications
- Better Star Ratings performance triggers quality bonus payments
- Reduced care team administrative burden lowers operational costs
For a Medicare Advantage plan with 50,000 members and 5,000 high-risk patients enrolled in care management, a $1,000 per patient cost reduction yields $5M in annual savings—substantially more than Health Cloud implementation and operational costs.
5. Patient Satisfaction and Engagement
Measurable Impact:
- 12-18 point improvement in CAHPS medication management questions
- 30-40% increase in patient portal medication list reviews
- 25-35% higher patient participation in care planning
Why This Happens:
- Patients receive consistent information from all providers (reducing confusion)
- Medication instructions are clear, personalized, and accessible via patient portal/mobile
- Patients feel heard when affordability and side effect concerns trigger coordinated responses
- Simplified medication regimens are easier to follow
Healthcare Use Cases: Medication Management in Action
Use Case 1: Medicare Advantage Star Ratings Improvement
Challenge: A 200,000-member Medicare Advantage plan struggled with Star Ratings measures related to medication adherence, particularly for diabetes, hypertension, and cholesterol medications (Part D measures).
Health Cloud Implementation:
- Integrated pharmacy claims data to calculate daily PDC for key medication classes
- Built risk stratification model identifying members likely to become non-adherent
- Created automated outreach campaigns via phone, email, and mail for members approaching adherence gaps
- Developed care coordinator workflows for high-risk members with barriers to adherence
Results:
- Diabetes medication adherence improved from 3 stars (75% adherent members) to 4.5 stars (88% adherent)
- Hypertension medication adherence improved from 3.5 stars to 5 stars (93% adherent)
- Star Ratings improvement triggered $8.2M in quality bonus payments
- 22% reduction in emergency department visits among intervention cohort
Use Case 2: Health System Care Transitions Program
Challenge: A 6-hospital integrated health system faced high readmission rates, with medication-related issues contributing to 35% of 30-day readmissions.
Health Cloud Implementation:
- Integrated discharge data from Epic EHR to identify all discharged patients
- Built 72-hour post-discharge medication reconciliation workflows
- Connected retail pharmacy data feeds to monitor prescription fills
- Created patient engagement tools for medication questions and concerns
Results:
- 30-day all-cause readmission rate decreased from 16.8% to 13.2%
- Medication-related readmissions decreased by 48%
- Medication reconciliation completion within 72 hours improved from 34% to 89%
- Care coordinator capacity to manage patients increased 35% through automation
Use Case 3: Specialty Pharmacy Care Coordination
Challenge: A specialty pharmacy managing complex chronic conditions (oncology, rheumatology, multiple sclerosis) struggled with coordinating care across multiple specialists, ensuring adherence to high-cost medications, and managing side effects.
Health Cloud Implementation:
- Created comprehensive patient profiles integrating medical, pharmacy, and lab data
- Built clinical pharmacist workflows for medication therapy management
- Developed side effect tracking and intervention protocols
- Integrated patient-reported outcomes for medication tolerability
Results:
- Medication adherence for specialty medications improved from 68% to 87%
- Average time to side effect identification and intervention reduced from 12 days to 3 days
- Patient satisfaction scores increased from 7.2 to 9.1 (out of 10)
- Clinical pharmacist productivity increased 40% (managing more patients with same staff)
Use Case 4: Accountable Care Organization (ACO) Medication Management
Challenge: A 45-practice ACO needed to coordinate medication management across independent physician practices with different EHR systems to improve quality scores and reduce total cost of care.
Health Cloud Implementation:
- Aggregated medication data from 4 different EHR systems plus pharmacy claims
- Created normalized, longitudinal medication records for all ACO patients
- Built clinical decision support for evidence-based prescribing (generics, therapeutic alternatives)
- Enabled care coordinators to support medication management across practice boundaries
Results:
- Generic dispensing rate improved from 82% to 91%
- Potentially inappropriate medications for elderly patients (Beers Criteria) reduced by 42%
- Total cost of care decreased $847 per patient per year
- ACO achieved shared savings for first time ($3.2M distribution)
Implementation Challenges and Practical Considerations
Health Cloud medication management capabilities are powerful, but implementation isn’t without challenges. Organizations achieve better outcomes when they approach these honestly and proactively.
Data Quality and Master Data Management
Challenge: Garbage in, garbage out. Medication data from multiple sources often contains:
- Inconsistent medication naming (brand vs. generic, abbreviations, misspellings)
- Missing dosage or frequency information
- Outdated medication statuses (discontinued medications still showing as active)
- Duplicate entries that automated deduplication can’t confidently resolve
Practical Approach:
- Invest in data quality assessment before implementation (understand your baseline)
- Implement RxNorm normalization for all medication entries
- Build human-in-the-loop workflows for ambiguous matching scenarios
- Create ongoing data stewardship processes, not just one-time cleanup
- Set realistic expectations—aim for 90-95% automated accuracy, not 100%
Integration Complexity
Challenge: Healthcare integration is notoriously difficult:
- Legacy systems with limited API capabilities
- Inconsistent FHIR implementations across vendors
- Varying data refresh frequencies (real-time vs. batch)
- Network and security constraints for data exchange
Practical Approach:
- Prioritize integrations by business value (start with highest-impact data sources)
- Use healthcare integration specialists (not general Salesforce consultants without healthcare experience)
- Plan for middleware/integration platforms (MuleSoft, Rhapsody) for complex scenarios
- Build monitoring and alerting for integration failures
- Document data lineage and refresh schedules clearly for end users
Workflow Adoption and Change Management
Challenge: Technology doesn’t improve outcomes—changed workflows performed by engaged users improve outcomes. Common adoption barriers include:
- Care coordinators comfortable with existing processes (even if inefficient)
- Physicians resistant to additional documentation requirements
- Concerns about workflow disruption during transition period
- Unclear value proposition for frontline staff
Practical Approach:
- Involve frontline users in workflow design from the beginning
- Focus on pain point elimination, not feature lists (“this saves you 45 minutes daily” not “look at this cool dashboard”)
- Provide role-based training with realistic patient scenarios
- Identify and empower clinical champions within departments
- Plan for parallel workflows during transition period
- Measure and communicate adoption metrics and outcome improvements
Regulatory and Compliance Considerations
Challenge: Medication management involves multiple regulatory requirements:
- HIPAA privacy and security requirements
- E-prescribing regulations (EPCS for controlled substances)
- State-specific pharmacy regulations
- Medicare and Medicaid documentation requirements
- Joint Commission medication reconciliation standards
Practical Approach:
- Engage compliance and legal teams early in planning
- Document all data access, sharing, and retention policies
- Implement appropriate role-based access controls
- Build audit trails for all medication changes
- Ensure e-prescribing integrations meet DEA requirements
- Plan for regular compliance audits
Clinical Decision Support Alert Fatigue
Challenge: Too many alerts lead to alert fatigue, where clinicians ignore warnings—including critical ones. Generic medication alerts often have poor specificity:
- Alerts for interactions that aren’t clinically significant in context
- Alerts for medications the patient isn’t actually taking
- Repetitive alerts for previously acknowledged issues
Practical Approach:
- Implement severity-based filtering (only surface high and moderate-severity alerts)
- Provide contextual information (why this alert matters for this specific patient)
- Allow appropriate alert dismissal with reason documentation
- Analyze alert override rates and refine rules
- Route different alert types to appropriate team members (pharmacist vs. physician vs. care coordinator)
Future Trends in Medication Management
Healthcare technology continues to evolve rapidly. Several emerging trends will shape the future of medication management in Health Cloud.
Artificial Intelligence and Predictive Analytics
Current State:
Today’s Health Cloud medication management relies primarily on rules-based logic—if X condition exists, then trigger Y alert.
Emerging Capabilities:
- Predictive non-adherence models: Machine learning algorithms analyzing patient characteristics, social determinants, past behavior, and medication complexity to predict which patients will struggle with adherence before they miss refills
- Personalized intervention recommendations: AI systems suggesting which intervention approach (phone call, text message, home visit, prescriber outreach) is most likely to succeed for specific patients based on historical response patterns
- Natural language processing for medication reconciliation: Extracting medication information from clinical notes, patient messages, and discharge summaries to auto-populate structured medication lists
- Drug efficacy prediction: Pharmacogenomic data combined with patient characteristics to predict which medications will be most effective and best tolerated
Health Cloud Integration Path:
Einstein AI platform capabilities increasingly integrated with Health Cloud enable custom predictive models trained on organization-specific data, with predictions surfaced directly in care coordinator workflows.
Internet of Medical Things (IoMT) Integration
Current State:
Medication adherence tracking relies primarily on pharmacy fill data (delayed indicator) and patient self-reporting (unreliable).
Emerging Capabilities:
- Smart medication dispensers: Connected pill boxes that track when medications are removed and send adherence data to Health Cloud
- Digital pills: Ingestible sensors that confirm medication consumption
- Smart insulin pens: Capturing insulin administration data for diabetic patients
- Wearable devices: Monitoring physiologic responses to medication (heart rate changes after beta-blocker administration, activity levels after COPD medication, etc.)
Health Cloud Integration Path:
IoMT device data flows into Health Cloud via FHIR Device and Observation resources, triggering workflow automation when adherence issues detected. Real-time physiologic data enables faster intervention for medication side effects or ineffectiveness.
Predictive Care and Preemptive Intervention
Current State:
Most medication management is reactive—identifying problems after they occur (missed refills, drug interactions when new medications prescribed).
Emerging Capabilities:
- Proactive deprescribing: Identifying medications that may no longer be necessary based on resolved conditions, changed circumstances, or emerging risks
- Predictive drug interaction detection: Anticipating future interactions based on typical treatment pathways for patient’s conditions
- Medication optimization algorithms: Continuously evaluating regimens for opportunities to simplify, reduce side effects, or improve efficacy
- Social determinants integration: Identifying patients at risk for adherence issues due to food insecurity, transportation challenges, or housing instability before medications are prescribed
Health Cloud Integration Path:
Integration between Health Cloud and population health analytics platforms enables risk stratification at scale, with highest-risk patients surfaced to care teams for proactive outreach.
Blockchain for Medication Supply Chain
Current State:
Medication data travels through multiple systems (prescriber, pharmacy, PBM, payer) with limited transparency and frequent reconciliation challenges.
Emerging Capabilities:
- Distributed ledger for prescription history: Immutable record of medication prescriptions, fills, and transfers accessible to all authorized parties
- Counterfeit medication prevention: Blockchain-verified medication authenticity from manufacturer to patient
- Controlled substance tracking: Enhanced monitoring for opioid prescriptions across provider networks
Health Cloud Integration Path:
Health Cloud could function as the interface layer to blockchain medication networks, presenting verified medication histories within familiar care team workflows while maintaining blockchain integrity in the background.
Voice and Conversational Interfaces
Current State:
Medication information is primarily accessed through traditional screens and keyboards.
Emerging Capabilities:
- Voice-enabled medication review: Care coordinators dictating medication reconciliation findings rather than typing
- Patient voice assistants: “Alexa, what medications do I take in the morning?” with information pulled from Health Cloud
- Conversational AI for medication questions: Patients asking medication questions via chatbot with escalation to pharmacists for complex issues
Health Cloud Integration Path:
Einstein Bots and voice integration capabilities enable conversational interfaces layered on top of Health Cloud medication data, with interactions documented back into patient timeline.
Conclusion: Strategic Considerations for Medication Management in Salesforce Health Cloud
Medication management in Salesforce Health Cloud represents a fundamental shift from fragmented, system-centric medication data to unified, patient-centric medication intelligence. For healthcare organizations, the question isn’t whether to improve medication management—the clinical and financial imperatives are clear. The question is how to do so effectively.
Health Cloud offers several strategic advantages:
Platform Approach: Rather than single-purpose medication management software, Health Cloud provides medication capabilities within a broader care coordination platform, eliminating the need for separate systems for different care management functions.
Healthcare Data Standards Alignment: FHIR-based data models ensure compatibility with modern healthcare IT ecosystems and future-proof implementations as interoperability standards evolve.
Configurability Without Custom Code: Healthcare workflows vary significantly across organizations. Health Cloud’s low-code configuration capabilities allow workflow customization without extensive custom development.
Ecosystem and Integration: The Salesforce AppExchange offers healthcare-specific applications extending medication management capabilities, while robust APIs enable integration with clinical systems.
Scalability: The Salesforce Platform handles implementations ranging from small physician practices to national health plans with millions of members.
Implementation Success Factors
Organizations achieving the best outcomes with Health Cloud medication management share common approaches:
- Start with specific use cases, not boil-the-ocean implementations: Focus first on highest-value scenarios (post-discharge reconciliation, high-risk medication adherence, etc.) and expand from there.
- Prioritize integration strategy: Health Cloud’s value is directly proportional to the quality and completeness of integrated data. Invest appropriately in integration architecture.
- Design workflows with frontline users: Technology teams can build systems, but frontline care coordinators, pharmacists, and physicians know where current processes break down.
- Plan for ongoing optimization: Initial implementation establishes the foundation; continuous improvement based on utilization data and outcomes measurements drives sustained value.
- Measure what matters: Track clinical outcomes (adherence rates, adverse events, readmissions) and operational metrics (care coordinator efficiency, reconciliation completion rates) alongside adoption metrics.
Is Health Cloud Right for Your Medication Management Needs?
Health Cloud medication management fits best for organizations that:
- Operate care management or care coordination programs where medication management is a core function
- Manage populations across multiple care settings requiring medication reconciliation
- Need to coordinate medication management across multiple provider organizations or care team members
- Require integration between clinical medication data and patient engagement tools
- Operate in value-based care models where medication adherence impacts quality metrics and financial outcomes
Health Cloud may be overbuilt for organizations that:
- Need only basic medication list functionality within a single clinical system
- Lack integration capabilities or resources to connect relevant data sources
- Have no care coordination function requiring cross-setting medication visibility
- Focus exclusively on episodic care rather than longitudinal population management
Final Perspective
Medication management isn’t a technology problem—it’s a coordination problem that technology can help solve. Salesforce Health Cloud provides the platform, integration capabilities, and workflow automation tools to enable effective coordination. However, technology alone doesn’t prevent medication errors, improve adherence, or reduce costs.
Success requires combining Health Cloud’s technical capabilities with well-designed clinical workflows, engaged care teams, appropriate resource allocation, and sustained organizational commitment to medication safety and therapeutic optimization.
For healthcare organizations serious about improving medication management—and willing to invest in the change management, integration work, and workflow redesign required—Health Cloud offers a comprehensive, scalable platform capable of delivering measurable clinical and financial outcomes.
The medication errors, adverse events, and preventable hospitalizations that occur today aren’t inevitable. They’re solvable problems. Health Cloud provides healthcare organizations with powerful tools to solve them—if implemented thoughtfully and used effectively.
About RizeX Labs
At RizeX Labs, we specialize in delivering advanced healthcare solutions powered by Salesforce Health Cloud. Our expertise combines deep technical knowledge, healthcare industry best practices, and real-world implementation experience to help organizations improve patient care, streamline operations, and ensure compliance.
We empower healthcare providers, payers, and life sciences organizations to transform fragmented systems into unified, intelligent care platforms—enabling personalized patient engagement, coordinated care, and better health outcomes.
Internal Linking Opportunities:
External Linking Opportunities:
- Salesforce official website
- Salesforce Health Cloud overview
- Salesforce documentation
- Salesforce AppExchange
- Healthcare interoperability standard (FHIR)
- HIPAA compliance guidelines
- MuleSoft (for healthcare integrations)
Quick Summary
Salesforce Health Cloud is a powerful healthcare CRM platform designed to provide a 360-degree view of patients, enabling organizations to deliver personalized, connected, and proactive care. It integrates clinical and non-clinical data from multiple systems, helping care teams make informed decisions faster.
With Health Cloud, healthcare organizations can improve patient engagement, enhance care coordination, ensure regulatory compliance, and reduce operational inefficiencies. As the healthcare ecosystem becomes more data-driven, adopting Health Cloud is essential for delivering modern, patient-centric care at scale.


