Introduction: The Shift to Proactive, Data-Driven Care
Healthcare delivery is experiencing a fundamental transformation. The traditional episodic care model—where patients visit providers only when symptoms emerge—is giving way to continuous, proactive monitoring. This shift isn’t merely technological; it’s a response to mounting pressures: rising chronic disease prevalence, aging populations, healthcare workforce shortages, and escalating costs.

Remote Patient Monitoring (RPM) addresses these challenges head-on. When integrated with Salesforce Health Cloud, Remote Patient Monitoring transcends simple data collection, evolving into an intelligent, actionable care delivery platform. For healthcare organizations already invested in the Salesforce ecosystem, this integration eliminates data silos, streamlines workflows, and transforms raw biometric data into meaningful clinical interventions.
The business case is compelling: organizations implementing Remote Patient Monitoring Salesforce solutions report 30-50% reductions in hospital readmissions, 20-38% decreases in emergency department visits, and improved patient satisfaction scores. More importantly, they’re achieving what matters most—better clinical outcomes through timely intervention.
Understanding Remote Patient Monitoring: Beyond Basic Definitions
Remote Patient Monitoring represents a structured healthcare delivery approach where digital technologies capture patient-generated health data (PGHD) outside traditional clinical settings. This data flows continuously to care teams who analyze, interpret, and act upon it.
RPM differs fundamentally from telehealth. While telehealth facilitates virtual consultations, RPM involves systematic, automated data transmission from connected devices—glucose monitors, blood pressure cuffs, pulse oximeters, wearables, and specialized sensors—directly into clinical workflows.
Critical RPM components include:
- Connected medical devices transmitting FDA-approved physiological data
- Secure data transmission infrastructure meeting HIPAA compliance standards
- Clinical analytics platforms identifying actionable patterns
- Care team workflows enabling timely interventions
- Patient engagement tools maintaining adherence and communication
The value emerges not from monitoring alone, but from converting continuous data streams into proactive interventions before acute episodes occur.
How RPM Works with Salesforce Health Cloud: Architecture and Integration
Salesforce Health Cloud provides the foundational patient relationship management infrastructure, while Remote Patient Monitoring capabilities transform it into a dynamic care coordination platform. This integration creates a comprehensive view of each patient, merging clinical data, device readings, social determinants, and care team communications into a unified interface.
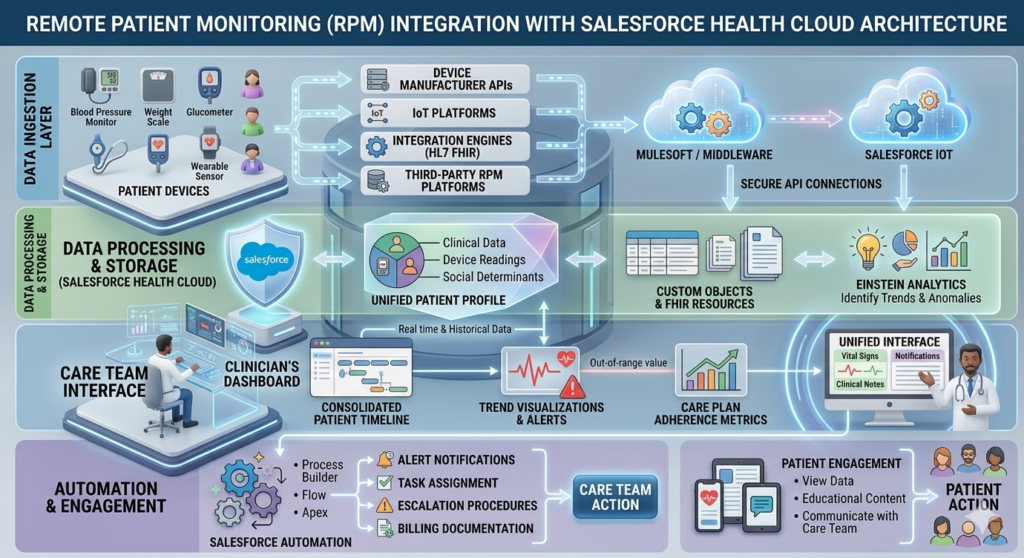
Integration Architecture
RPM Health Cloud implementations typically follow this technical architecture:
Data Ingestion Layer: IoT Healthcare Salesforce integrations leverage APIs, HL7 FHIR standards, and middleware platforms to ingest device data. Popular integration patterns include:
- Direct API connections to device manufacturers (e.g., Omron, iHealth, Withings)
- IoT platforms like Salesforce IoT Cloud creating device events
- Healthcare integration engines (Mirth Connect, Rhapsody) normalizing data streams
- Third-party RPM platforms (Vivify Health, 100Plus) with pre-built Health Cloud connectors
Data Processing and Storage: Incoming device readings populate custom Health Cloud objects or standard FHIR resources. Salesforce’s Einstein Analytics processes this data, applying algorithms to identify trends, anomalies, and threshold violations.
Care Team Interface: Providers access consolidated patient timelines displaying:
- Real-time and historical device readings with trend visualization
- Alert notifications for out-of-range values
- Care plan adherence metrics
- Communication history and clinical notes
- Scheduled interventions and follow-ups
Patient Engagement: Connected Healthcare Salesforce solutions extend to patient-facing portals and mobile applications where individuals view their own data, receive educational content, and communicate with care teams.
Workflow Automation
Salesforce’s automation capabilities—Process Builder, Flow, and Apex—enable sophisticated clinical workflows:
- Automated alerts when readings exceed defined thresholds
- Assignment rules routing cases to appropriate care team members
- Escalation procedures for critical values requiring immediate intervention
- Automated patient outreach via SMS, email, or in-app notifications
- Documentation requirements triggering when billing criteria are met
This automation reduces administrative burden while ensuring no critical data point goes unnoticed.
Key Features: What Sets Health Cloud RPM Apart
1. 360-Degree Patient View
Health Cloud’s foundational architecture consolidates disparate data sources—EHR systems, claims data, RPM devices, social determinants—into a comprehensive patient profile. Care coordinators access complete context before every intervention.
2. Intelligent Alert Management
Not all data points warrant clinical attention. Health Cloud’s configurable alert logic applies patient-specific thresholds, trending algorithms, and clinical rules to distinguish signal from noise. This reduces alert fatigue while ensuring genuine concerns receive immediate attention.
3. Care Plan Orchestration
RPM data directly informs care plan adjustments. When readings indicate deterioration, automated workflows can:
- Modify medication schedules
- Trigger nurse check-ins
- Schedule provider appointments
- Initiate care team collaboration
4. Regulatory Compliance and Billing Integration
RPM reimbursement requires specific documentation: device provision, patient consent, monitoring time, and intervention records. Health Cloud tracks these requirements automatically, triggering billing workflows when CPT code criteria are met (99453, 99454, 99457, 99458).
5. Multi-Tenant Collaboration
Comprehensive care requires coordination across providers, specialists, caregivers, and patients themselves. Health Cloud’s collaboration tools ensure all stakeholders access appropriate information while maintaining security boundaries.
6. Predictive Analytics
Einstein Analytics applies machine learning to historical RPM data, identifying patients at high risk for adverse events. These predictive insights enable preemptive interventions before crises develop.
Business Benefits: Measurable Impact on Operations and Outcomes
Reduced Hospital Readmissions
The financial impact of readmissions is substantial—CMS penalizes hospitals with excessive 30-day readmission rates. RPM Health Cloud implementations demonstrate measurable improvements:
- Heart failure programs: 38-44% readmission reduction
- COPD monitoring: 30-35% decrease in hospital returns
- Post-surgical monitoring: 25-30% reduction in complications requiring readmission
Financial impact: For a 300-bed hospital with annual readmission penalties of $500,000, a 35% improvement translates to $175,000 in avoided penalties, plus the marginal cost savings of prevented readmissions (averaging $12,000-15,000 per event).
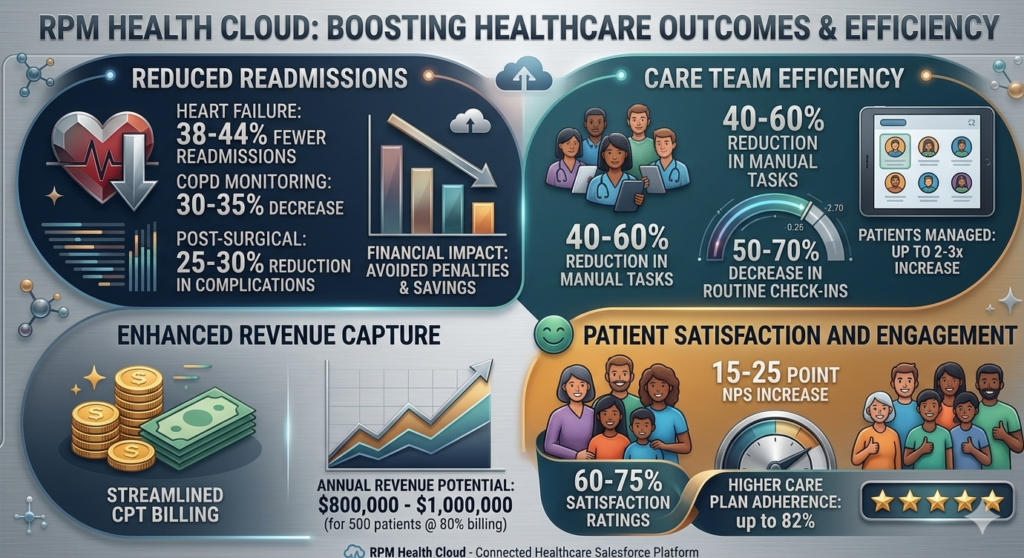
Improved Care Team Efficiency
Connected Healthcare Salesforce platforms eliminate manual data entry and phone-based monitoring. Care coordinators manage larger patient panels while providing more personalized attention:
- 40-60% reduction in manual data collection time
- 50-70% decrease in routine check-in calls
- 2-3x increase in patients managed per care coordinator
Operational impact: A care coordinator previously managing 75 patients can effectively oversee 150-200 with RPM automation, dramatically improving program economics.
Enhanced Revenue Capture
RPM represents a legitimate reimbursement opportunity. Medicare and most commercial payers reimburse for qualified RPM services:
- Initial device setup and patient education (CPT 99453): ~$19
- Monthly device supply and data transmission (CPT 99454): ~$64
- First 20 minutes of monitoring/management (CPT 99457): ~$51
- Additional 20 minutes (CPT 99458): ~$41
For a program monitoring 500 chronic disease patients with 80% qualifying for full monthly billing, annual revenue potential approaches $800,000-1,000,000.
Patient Satisfaction and Engagement
Patients appreciate proactive monitoring that prevents health crises. Organizations report:
- 15-25 point increases in Net Promoter Scores
- 60-75% patient satisfaction ratings for RPM programs
- Higher care plan adherence rates (68-82% vs. 45-55% without monitoring)
Real-World Use Cases: RPM Health Cloud in Action
Case Study 1: Multispecialty Clinic Reduces Heart Failure Readmissions
A 12-clinic healthcare system implemented Remote Patient Monitoring Salesforce for their 800-patient heart failure population. Patients received connected scales and blood pressure monitors transmitting daily readings to Health Cloud.
Implementation approach:
- Integrated with Epic EHR for bidirectional data flow
- Configured alert thresholds based on ejection fraction and NYHA class
- Established tiered response protocols (nurse outreach, telehealth visit, ED referral)
- Created patient-specific dashboards accessible via mobile app
Results after 18 months:
- 42% reduction in 30-day readmissions
- 87% patient enrollment acceptance rate
- $2.1 million in avoided readmission costs
- 5.2:1 ROI including reimbursement and savings
The system particularly credited Health Cloud’s care plan integration—when weight gain exceeded thresholds, automated workflows adjusted diuretic protocols and triggered same-day nurse consultations before decompensation occurred.
Case Study 2: Accountable Care Organization Manages Diabetes at Scale
An ACO responsible for 45,000 Medicare lives targeted their 3,200 poorly controlled diabetics (HbA1c >9%) with an IoT Healthcare Salesforce program providing connected glucometers.
Implementation highlights:
- Leveraged Salesforce Community Cloud for patient portal
- Integrated Einstein Analytics to identify non-adherent patients
- Built automated educational content delivery based on reading patterns
- Created pharmacist-led intervention workflows for trending issues
Outcomes:
- Average HbA1c reduction of 1.4% across participant population
- 34% decrease in diabetes-related emergency visits
- Shared savings distribution of $1.8 million
- Quality measure improvement lifting MSSP performance tier
The ACO found that Salesforce’s segmentation capabilities allowed personalized interventions—recently diagnosed patients received different educational content and monitoring cadences than long-term diabetics with complications.
Case Study 3: Rural Health Network Extends Specialist Access
A rural health network spanning 400 miles implemented RPM Health Cloud to provide virtual cardiology and pulmonology support to remote primary care practices.
Program design:
- Primary care providers enrolled patients in remote monitoring
- Specialists at the hub hospital reviewed RPM data weekly
- Alert protocols enabled immediate specialist consultation
- Reduced need for patient travel to specialty appointments
Impact:
- 68% reduction in specialist appointment no-shows (eliminated travel barriers)
- Average patient travel savings of 180 miles per quarter
- Specialist capacity to serve 3x more patients
- Improved specialist-PCP collaboration and knowledge transfer
This model demonstrates how Connected Healthcare Salesforce platforms extend beyond monitoring to fundamentally reshape care delivery models in access-constrained environments.
Challenges and Limitations: Realistic Implementation Considerations
Technical Integration Complexity
Despite standardization efforts, healthcare technology integration remains challenging. Organizations face:
- Device manufacturer API variability and limitations
- EHR integration requiring HL7/FHIR expertise
- Data normalization across different device types
- Ongoing maintenance as platforms evolve
Mitigation: Partner with experienced Salesforce Health Cloud implementation consultants. Prioritize devices and platforms with established Health Cloud connectors. Budget 20-30% of project costs for integration development and testing.
Patient Adoption and Technology Literacy
Not all patients embrace connected devices. Barriers include:
- Limited digital literacy, particularly among elderly populations
- Connectivity challenges (inadequate WiFi, no smartphones)
- Device fatigue and monitoring adherence decline
- Privacy concerns about continuous data transmission
Mitigation: Implement tiered technology approaches (cellular-enabled devices for connectivity-challenged patients). Provide comprehensive onboarding with ongoing support. Be transparent about data usage and security. Accept that RPM isn’t appropriate for all patients—focus on those most likely to benefit and engage.
Alert Fatigue and Workflow Burden
Poorly configured RPM programs generate overwhelming alert volumes, leading care teams to ignore genuinely critical notifications.
Mitigation: Invest significant time in threshold configuration and alert logic refinement. Implement tiered alert systems (immediate attention vs. routine review). Continuously analyze alert patterns and adjust rules. Ensure adequate staffing to manage alert volumes—technology doesn’t reduce workforce needs, it redirects capacity toward higher-value activities.
Reimbursement Complexity and Documentation Requirements
While RPM reimbursement exists, capturing it requires meticulous documentation:
- 16 days of data transmission per month
- 20+ minutes of qualified interactive communication
- Physician or qualified healthcare professional oversight
- Proper consent documentation
Mitigation: Build billing compliance directly into Health Cloud workflows. Automated tracking of monitoring time, communication minutes, and documentation completeness ensures no revenue leakage. Regular billing audits identify gaps before claims submission.
Data Privacy and Security
RPM expands the attack surface for healthcare organizations. Device vulnerabilities, transmission security, and data storage must meet stringent requirements.
Mitigation: Leverage Salesforce’s HIPAA-compliant infrastructure. Implement BAAs with all device manufacturers and integration partners. Conduct regular security assessments. Ensure device firmware updates are deployed promptly.
Future Trends: The Evolution of RPM Health Cloud
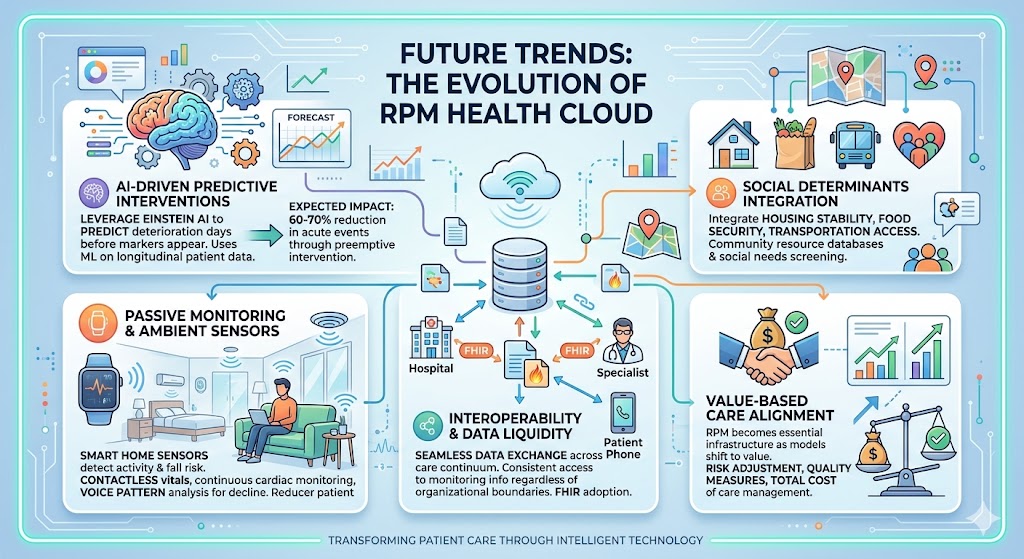
1. AI-Driven Predictive Interventions
Current RPM largely responds to threshold violations. Next-generation implementations will leverage Einstein AI to predict deterioration days before traditional markers appear. Machine learning models trained on longitudinal patient data will identify subtle pattern changes indicating impending exacerbations.
Expected impact: 60-70% reduction in acute events through preemptive intervention, not reactive response.
2. Social Determinants Integration
Health outcomes correlate more strongly with social factors—housing stability, food security, transportation access—than clinical interventions alone. Future RPM Health Cloud implementations will integrate:
- Community resource databases
- Social needs screening workflows
- Referral management to social services
- Outcome tracking across clinical and social interventions
This holistic approach addresses root causes, not just symptoms.
3. Passive Monitoring and Ambient Sensors
Current RPM requires active patient participation—remembering to take readings, transmit data, charge devices. Emerging technologies enable passive monitoring:
- Smart home sensors detecting activity patterns and fall risk
- Contactless vital sign monitoring through radar technology
- Wearables providing continuous cardiac monitoring without user interaction
- AI analysis of voice patterns indicating cognitive decline or respiratory issues
These technologies reduce patient burden while providing richer data streams.
4. Interoperability and Data Liquidity
FHIR adoption and interoperability mandates are making health data more portable. Future Connected Healthcare Salesforce implementations will seamlessly exchange RPM data across the care continuum—acute facilities, post-acute providers, specialists, and patients themselves maintain consistent access to monitoring information regardless of organizational boundaries.
5. Value-Based Care Alignment
As healthcare payment models shift from volume to value, RPM becomes essential infrastructure. Future implementations will directly tie to:
- Risk adjustment and hierarchical condition categories (HCC) optimization
- Quality measure performance
- Total cost of care management
- Population health stratification and intervention targeting
Health Cloud will evolve from a care coordination platform to a comprehensive value-based care operating system with RPM as a core capability.
Conclusion: Strategic Imperative for Forward-Thinking Healthcare Organizations
Remote Patient Monitoring in Salesforce Health Cloud represents more than incremental improvement—it’s a fundamental reimagining of how healthcare organizations engage patients, coordinate care, and demonstrate value. For healthcare systems already invested in Salesforce, RPM capabilities transform existing infrastructure into a dynamic, proactive care delivery platform.
The business case is clear: measurable reductions in acute care utilization, improved clinical outcomes, legitimate revenue opportunities, and enhanced competitive positioning. Organizations that master Connected Healthcare Salesforce implementations today are building the foundation for tomorrow’s value-based care requirements.
However, success requires more than technology deployment. It demands careful patient selection, thoughtful workflow design, continuous optimization, and genuine organizational commitment to care model transformation. RPM isn’t a project—it’s an ongoing program requiring sustained investment and attention.
For healthcare leaders evaluating RPM Health Cloud, begin with a focused pilot targeting a specific population where impact can be demonstrated quickly—heart failure, diabetes, or hypertension management. Prove the value proposition, refine workflows, build organizational confidence, then systematically expand.
The future of healthcare is proactive, data-driven, and patient-centered. Remote Patient Monitoring Salesforce solutions provide the practical pathway from aspiration to reality. Organizations that act decisively today will define the standard of care tomorrow.
About RizeX Labs
At RizeX Labs, we specialize in delivering advanced healthcare solutions powered by Salesforce Health Cloud. Our expertise combines deep technical knowledge, healthcare industry best practices, and real-world implementation experience to help organizations improve patient care, streamline operations, and ensure compliance.
We empower healthcare providers, payers, and life sciences organizations to transform fragmented systems into unified, intelligent care platforms—enabling personalized patient engagement, coordinated care, and better health outcomes.
Internal Linking Opportunities:
- Link to your Salesforce course page:
https://rizexlabs.com/salesforce-admin-and-development-training
External Linking Opportunities:
- Salesforce official website: https://www.salesforce.com/
- Salesforce Health Cloud overview: https://www.salesforce.com/products/health-cloud/overview/
- Salesforce documentation: https://help.salesforce.com/
- Salesforce AppExchange: https://appexchange.salesforce.com/
- Healthcare interoperability standard (FHIR): https://www.hl7.org/fhir/
- HIPAA compliance guidelines: https://www.hhs.gov/hipaa/index.html
- MuleSoft (for healthcare integrations): https://www.mulesoft.com/
Quick Summary
Salesforce Health Cloud is a powerful healthcare CRM platform designed to provide a 360-degree view of patients, enabling organizations to deliver personalized, connected, and proactive care. It integrates clinical and non-clinical data from multiple systems, helping care teams make informed decisions faster.
With Health Cloud, healthcare organizations can improve patient engagement, enhance care coordination, ensure regulatory compliance, and reduce operational inefficiencies. As the healthcare ecosystem becomes more data-driven, adopting Health Cloud is essential for delivering modern, patient-centric care at scale.
Quick Summary
Remote Patient Monitoring (RPM) in Salesforce Health Cloud represents a shift from reactive to proactive, data-driven healthcare by continuously collecting patient data through connected devices and transforming it into actionable insights for care teams. Integrated with Health Cloud, RPM eliminates data silos, automates workflows, and enables real-time interventions, leading to improved clinical outcomes, reduced hospital readmissions, enhanced care team efficiency, and new revenue opportunities. With features like predictive analytics, intelligent alerts, and comprehensive patient views, it empowers healthcare organizations to deliver personalized, coordinated care. However, successful implementation requires overcoming challenges such as integration complexity, patient adoption, and compliance. Ultimately, RPM is not just a technological upgrade but a strategic move toward value-based, patient-centered healthcare delivery.


