Introduction to 360-Degree Patient View
The 360-degree patient view in Salesforce Health Cloud represents a transformative approach to healthcare data management, providing clinicians, care coordinators, and healthcare professionals with a comprehensive, unified perspective of each patient’s complete health journey. This holistic view consolidates disparate data sources into a single, intuitive interface that empowers healthcare organizations to deliver personalized, coordinated care while improving patient outcomes and operational efficiency.
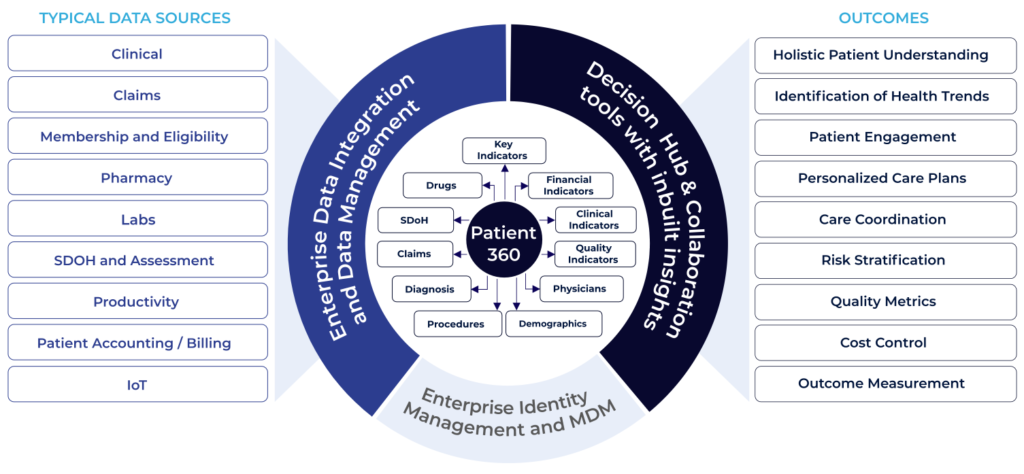
In today’s complex healthcare landscape, patient information is often fragmented across multiple systems, departments, and even organizations. Electronic Health Records (EHRs), laboratory systems, imaging platforms, pharmacy databases, and billing systems all contain critical pieces of the patient puzzle. The 360-degree patient view solves this challenge by aggregating this information into a unified dashboard that presents a complete picture of the patient’s medical history, current health status, social determinants of health, care team interactions, and treatment plans.
Salesforce Health Cloud leverages the power of the Salesforce platform—known for its customer relationship management capabilities—and specifically adapts it for healthcare use cases. The platform is built on industry standards like HL7 FHIR (Fast Healthcare Interoperability Resources), ensuring seamless integration with existing healthcare IT infrastructure while maintaining compliance with regulations such as HIPAA, GDPR, and other data privacy requirements.
Core Components of the 360-Degree Patient View
Patient Demographics and Identification
The foundation of any comprehensive patient view begins with accurate demographic information. Salesforce Health Cloud captures and displays essential patient identifiers including full legal name, date of birth, gender, social security number, medical record numbers (MRNs), insurance identification numbers, and contact information. The system supports multiple identifiers across different healthcare systems, which is particularly valuable for patients who receive care from multiple providers or health systems. This component also includes preferred language, communication preferences, emergency contacts, and authorized representatives or caregivers who may be involved in care decisions.
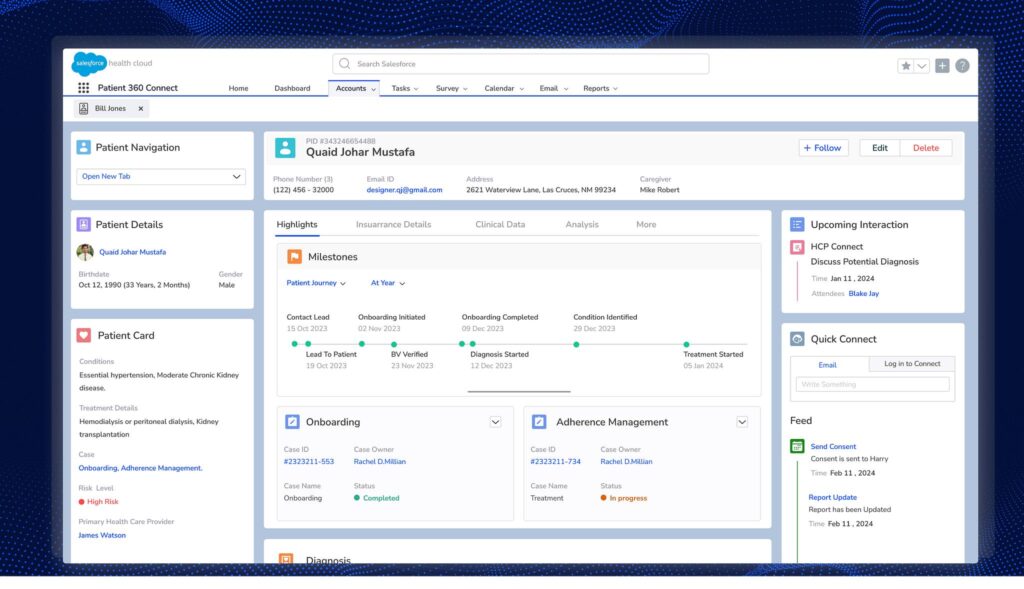
The demographic section extends beyond basic identification to include cultural and social factors that influence healthcare delivery. Information about the patient’s preferred communication methods, accessibility needs, religious beliefs that might impact care decisions, and cultural considerations are all captured to ensure culturally competent care delivery. The system also maintains a comprehensive address history, which can be valuable for tracking patient mobility and understanding environmental factors that might influence health outcomes.
Comprehensive Medical History
The medical history component provides an exhaustive timeline of the patient’s health journey. This includes past diagnoses, chronic conditions, acute illnesses, surgical histories, hospitalizations, and emergency department visits. Each condition is documented with relevant details including diagnosis dates, severity levels, current status (active, resolved, or in remission), and associated treatment plans. The system maintains both current active problems and historical conditions, allowing clinicians to understand not just the patient’s present health status but also their complete medical trajectory.
Allergies and adverse reactions constitute a critical safety component within the medical history. The 360-degree view prominently displays known allergies to medications, foods, environmental factors, and other substances. Each allergy entry includes the specific allergen, reaction type, severity level, and date of discovery. Clinical decision support systems leverage this information to provide real-time alerts when potentially harmful medications or treatments are being considered, significantly reducing the risk of adverse events.
Family medical history is integrated into the comprehensive view, documenting hereditary conditions, genetic predispositions, and familial health patterns that might inform preventive care strategies and screening recommendations. This information is particularly valuable for assessing risk factors for conditions with strong genetic components such as cardiovascular disease, certain cancers, diabetes, and hereditary disorders.
Medications and Treatment Plans
The medication management component provides a complete view of the patient’s current medications, past prescriptions, over-the-counter medications, supplements, and herbal remedies. Each medication entry includes the drug name, dosage, frequency, route of administration, prescribing physician, start date, end date (if applicable), and refill information. The system tracks medication adherence by integrating with pharmacy systems and patient-reported data, identifying potential compliance issues that might require intervention from care teams.
Drug interaction checking is embedded within this component, automatically screening for potential interactions between prescribed medications, contraindications based on patient allergies or conditions, and duplicative therapies. Advanced decision support algorithms alert clinicians to potential issues before prescriptions are finalized, improving patient safety and reducing adverse drug events.
Treatment plans extend beyond medications to encompass all therapeutic interventions including physical therapy, occupational therapy, dietary modifications, lifestyle recommendations, and scheduled procedures. Each treatment plan element is documented with clear objectives, timelines, responsible providers, and progress tracking mechanisms. Care teams can monitor adherence to treatment plans and adjust interventions based on patient progress and outcomes.
Clinical Encounters and Care Timeline
The care timeline presents a chronological view of all patient interactions with the healthcare system. This includes office visits, hospital admissions, emergency department encounters, telehealth appointments, telephone consultations, and care coordination contacts. Each encounter is documented with the date, location, attending providers, chief complaint, diagnoses, procedures performed, and clinical notes. This timeline view allows clinicians to quickly understand the frequency and nature of patient engagement with the healthcare system, identifying patterns that might indicate deteriorating conditions, effective interventions, or opportunities for preventive care.
Integration with clinical documentation systems ensures that provider notes, nursing assessments, and multidisciplinary team observations are accessible within the 360-degree view. Natural language processing capabilities can extract key clinical insights from unstructured notes, making critical information more discoverable and actionable. The timeline can be filtered by encounter type, provider, location, or condition, enabling users to focus on specific aspects of the patient’s care history.
Diagnostic Results and Clinical Data
Laboratory results, imaging studies, pathology reports, and other diagnostic findings are integrated into the patient view with trending capabilities that allow clinicians to visualize changes over time. Laboratory values are displayed with reference ranges, abnormal flags, and historical comparisons that help identify emerging issues or improvement trends. Graphical representations of key metrics like hemoglobin A1C for diabetic patients, blood pressure readings for hypertensive patients, or tumor markers for oncology patients provide intuitive visualization of disease progression or treatment response.
Imaging study results are accessible with links to the actual images through PACS (Picture Archiving and Communication System) integration. Radiology reports, interpretations, and comparison studies are available within the same interface, eliminating the need to navigate multiple systems. Critical results are flagged and routed to appropriate providers through automated notification systems, ensuring timely clinical response to abnormal findings.
Care Team and Provider Network
Healthcare is inherently collaborative, and the 360-degree patient view reflects this reality by displaying the complete care team involved in each patient’s care. This includes primary care physicians, specialists, nurses, care coordinators, social workers, pharmacists, dietitians, mental health professionals, and community health workers. Each team member’s role, contact information, and specific responsibilities are documented, facilitating communication and care coordination.
The care team view shows not just current providers but also historical relationships, which can be valuable when coordinating care or seeking input from clinicians who have previously treated the patient. Referral relationships are tracked, showing which providers referred the patient to specialists and the status of those referrals. This visibility helps prevent duplicate referrals, identify gaps in specialist care, and ensure appropriate follow-up after specialist consultations.
Insurance and Financial Information
Financial information is integrated into the patient view to support informed decision-making about treatment options and care planning. Insurance coverage details including primary and secondary insurance, coverage periods, authorization requirements, and benefits information are readily accessible. This enables care teams to consider financial implications when recommending treatments and helps identify patients who might benefit from financial assistance programs or alternative care pathways.
Prior authorization tracking shows which procedures or medications require pre-approval from insurance companies, the status of authorization requests, and approval or denial decisions. This visibility helps prevent delays in care delivery and enables proactive outreach to patients when authorizations are pending or denied. Outstanding balances, payment plans, and financial assistance enrollments are also visible, allowing care coordinators to address financial barriers that might impact care adherence.
Social Determinants of Health
Recognizing that health outcomes are influenced by factors beyond clinical care, the 360-degree patient view incorporates social determinants of health (SDOH) data. This includes information about housing stability, food security, transportation access, employment status, education level, social support networks, and exposure to violence or trauma. Understanding these contextual factors enables care teams to address root causes of health inequities and connect patients with community resources that support health and well-being.
SDOH screening tools are embedded within the platform, allowing care teams to systematically assess patient needs across multiple domains. Responses to screening questions are stored and tracked over time, enabling monitoring of changing social circumstances that might impact health. Integration with community resource databases facilitates referrals to social services, food banks, housing assistance programs, transportation services, and other supports.
Patient Engagement and Communication History
The communication history component tracks all interactions between patients and the healthcare organization across multiple channels. This includes phone calls, emails, text messages, patient portal messages, mail correspondence, and in-person conversations. Understanding communication patterns helps care teams identify engaged patients versus those who might benefit from more proactive outreach. The system also tracks patient preferences for communication timing, channels, and frequency, enabling personalized engagement strategies.
Patient-generated health data from wearable devices, home monitoring equipment, symptom trackers, and patient-reported outcomes are integrated into the view. This real-world data provides insights into patient health status between clinical encounters, enabling early identification of deteriorating conditions and supporting remote monitoring programs. Trends in patient-generated data can trigger automated alerts to care teams when values fall outside acceptable parameters.
Goals and Care Plans
Patient-centered care planning is supported through documentation of patient health goals, care plan elements, and progress toward objectives. Goals might include clinical targets like achieving specific blood pressure or blood sugar levels, functional objectives like improving mobility or managing pain, or behavioral goals like increasing physical activity or smoking cessation. Each goal is documented with specific, measurable targets, timelines, and assigned responsibilities among care team members.
Care plans outline the interventions, services, and supports designed to help patients achieve their goals. Plans are developed collaboratively with patients and families, incorporating their preferences, values, and priorities. Progress toward goals is tracked through regular assessments, with care plans adjusted based on patient response and changing circumstances. This component supports value-based care models by maintaining focus on outcomes that matter most to patients.
Technical Architecture and Integration Capabilities
FHIR Integration Standards
Salesforce Health Cloud is built on HL7 FHIR standards, the emerging global standard for healthcare interoperability. FHIR resources represent discrete healthcare concepts like patients, encounters, observations, medications, and conditions in a standardized data format. This standards-based approach enables the platform to exchange data with external systems regardless of vendor, creating a truly interoperable healthcare ecosystem. FHIR APIs facilitate real-time data exchange, allowing the 360-degree patient view to remain current with information from connected systems.
The platform supports multiple FHIR versions and implementation guides, accommodating the varying maturity levels of different healthcare IT systems. Mapping engines translate between different data standards and formats, normalizing information from diverse sources into a consistent representation within the patient view. This technical foundation ensures that data from EHRs, laboratories, imaging systems, health information exchanges, and other sources can be seamlessly incorporated into the comprehensive patient profile.
Data Security and Privacy Controls
Healthcare data is among the most sensitive information organizations manage, and Salesforce Health Cloud incorporates robust security and privacy controls to protect patient information. Role-based access controls ensure that users can only view information appropriate to their role and relationship with specific patients. Audit logging tracks all access to patient records, creating an accountability trail that supports compliance audits and security investigations.
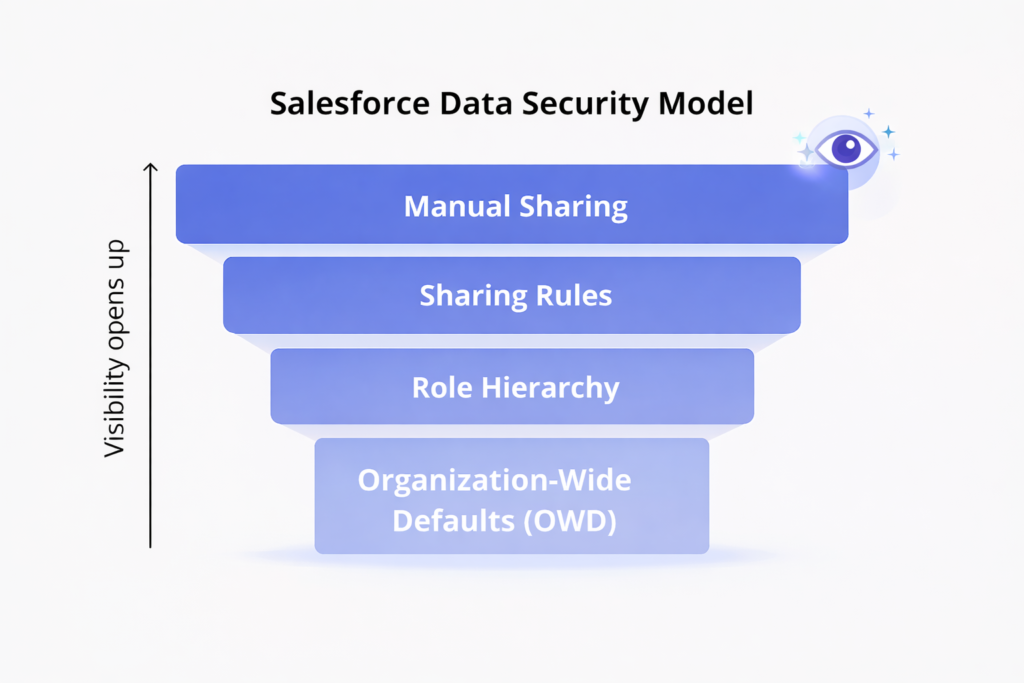
Data encryption protects information both at rest and in transit, ensuring that patient data remains secure as it moves between systems and when stored in databases. De-identification capabilities support research and analytics use cases by removing personally identifiable information while preserving the clinical utility of data. Consent management features enable patients to control who can access their information and for what purposes, supporting patient privacy preferences and regulatory requirements like GDPR.
EHR Integration Approaches
While Health Cloud provides a comprehensive patient view, it typically operates alongside rather than replacing existing EHR systems. Integration with EHRs is accomplished through various technical approaches including FHIR APIs, HL7 v2 messaging, proprietary APIs, and data extracts. The integration strategy depends on the specific EHR system, organizational requirements, and use cases being supported.
Bi-directional integration enables data flow in both directions, allowing updates made in Health Cloud to be reflected back in source systems and vice versa. This synchronization ensures data consistency across platforms and prevents the creation of information silos. Real-time integration supports clinical decision-making with current information, while batch integration processes might be used for historical data loading and less time-sensitive updates.
Analytics and Artificial Intelligence
The platform incorporates analytics capabilities that transform raw patient data into actionable insights. Population health analytics identify cohorts of patients with similar characteristics, conditions, or risk factors, enabling targeted interventions and preventive programs. Predictive analytics leverage machine learning algorithms to forecast patient outcomes, identify high-risk individuals, and recommend interventions likely to improve results.

Natural language processing extracts structured information from unstructured clinical notes, radiology reports, and other text-based documents. Sentiment analysis can identify patients expressing frustration, confusion, or satisfaction in their communications, enabling appropriate responses. Computer vision capabilities might be applied to analyze medical images or photographs captured by patients using smartphone apps.
Einstein AI, Salesforce’s artificial intelligence platform, provides intelligent recommendations to care teams based on patterns identified across patient populations. These might include suggested care plan elements for patients with specific conditions, optimal communication timing and channels for individual patients, or identification of patients likely to benefit from specific programs or interventions.
Key Use Cases and Applications
Chronic Disease Management
Chronic conditions like diabetes, heart disease, chronic obstructive pulmonary disease, and chronic kidney disease require ongoing monitoring, patient engagement, and care coordination. The 360-degree patient view supports chronic disease management by consolidating all relevant clinical data, enabling care teams to monitor disease progression, track adherence to treatment plans, and intervene proactively when metrics suggest deteriorating control.
Disease-specific dashboards present key indicators in an intuitive format. For diabetic patients, this might include hemoglobin A1C trends, blood glucose readings, medication adherence, diabetes education completion, annual eye exam status, and foot exam compliance. Care coordinators can identify patients falling behind on recommended care and reach out with appointment reminders, education, or motivational support. The platform can automate some outreach based on predefined rules, ensuring consistent engagement while allowing care teams to focus on patients with the most complex needs.
Care Coordination and Transitions of Care
Care transitions between settings—hospital to home, hospital to skilled nursing facility, or primary care to specialty care—represent vulnerable periods when patients face increased risk of adverse events, medication errors, and readmissions. The 360-degree patient view improves care transitions by ensuring that receiving providers have complete, accurate information about the patient’s hospital course, discharge medications, follow-up requirements, and pending tests or consultations.
Transition checklists can be configured for different care scenarios, ensuring that all necessary elements are completed before discharge or transfer. Automated notifications alert receiving providers about incoming patients, and care coordinators can monitor completion of post-discharge requirements like follow-up appointments and medication reconciliation. This comprehensive visibility and workflow support reduces readmissions, improves patient safety, and enhances the patient experience during transitions.
Population Health Management
Beyond individual patient care, the 360-degree patient view supports population health initiatives by enabling identification and management of patient cohorts. Quality measure reporting is streamlined through automated calculation of metrics like cancer screening rates, immunization coverage, blood pressure control in hypertensive patients, and diabetes care quality indicators. Gaps in care are automatically identified, allowing outreach to patients who are overdue for screenings, vaccinations, or preventive services.
Risk stratification algorithms assign patients to different risk tiers based on clinical, functional, and social factors. High-risk patients might be enrolled in intensive care management programs with frequent contact from care coordinators, while lower-risk patients receive less intensive monitoring. Resource allocation is optimized by matching intervention intensity to patient need, improving outcomes while managing costs.
Value-Based Care and Quality Reporting
As healthcare organizations increasingly participate in value-based payment models, the 360-degree patient view provides essential infrastructure for success in these arrangements. Attribution logic assigns patients to specific providers or care teams, establishing accountability for outcomes and costs. Quality metrics aligned with specific value-based contracts are tracked automatically, with dashboards showing performance against targets and financial implications of results.
Care gaps that impact quality scores or financial performance are identified at both individual and population levels. Provider performance dashboards show how individual clinicians or care teams are performing on key metrics, supporting accountability and continuous improvement. Documentation completeness checks ensure that all qualifying care activities are properly captured for reporting purposes.
Patient Engagement and Empowerment
Patient portals integrated with Health Cloud provide patients access to their own 360-degree view, albeit with presentation and terminology appropriate for consumers rather than clinicians. Patients can review their medical history, medications, test results, and upcoming appointments. Educational resources relevant to their specific conditions and care plans are delivered through the portal, supporting informed decision-making and self-management.
Secure messaging enables convenient communication between patients and care teams for non-urgent questions, medication refill requests, and appointment scheduling. Appointment reminders delivered through patients’ preferred channels (email, text, phone) reduce no-shows and improve care continuity. Online appointment scheduling gives patients control over when and where they receive care, improving satisfaction and engagement.
Implementation Considerations and Best Practices
Data Governance and Quality
The value of a 360-degree patient view depends entirely on the quality, completeness, and accuracy of the underlying data. Organizations implementing Health Cloud must establish robust data governance frameworks that define data ownership, quality standards, validation rules, and stewardship responsibilities. Master data management processes ensure consistent representation of patients, providers, locations, and other key entities across integrated systems.
Data quality monitoring should be continuous, with automated checks identifying incomplete records, inconsistent values, or outdated information. Duplication detection and resolution processes prevent creation of multiple records for the same patient, which fragments the view and creates safety risks. Data stewards from clinical and operational departments should be engaged in ongoing quality improvement efforts, using dashboard metrics to identify and address systematic data issues.
Change Management and User Adoption
Technology alone does not transform care delivery—people and processes must evolve as well. Successful Health Cloud implementations require comprehensive change management programs that prepare users for new workflows, build competencies with new tools, and create enthusiasm for improved capabilities. Stakeholder engagement beginning in the planning phases ensures that system configuration aligns with actual clinical workflows and user needs.
Training programs should be role-specific and scenario-based, allowing users to practice realistic activities they will perform in production. Super users from key departments can serve as department champions, providing peer support and feedback to implementation teams. Go-live support with extra resources available to answer questions and resolve issues helps ensure smooth transitions. Post-implementation, ongoing training for new users and refresher sessions for existing users maintain and build competencies.
Workflow Integration and Clinical Decision Support
The 360-degree patient view should be integrated into existing clinical workflows rather than requiring users to navigate to a separate system for specific tasks. Single sign-on capabilities reduce authentication friction, and context-aware launching allows users to open the patient view directly to a specific patient context from EHRs or other applications. Embedded analytics and decision support provide insights and recommendations at the point of care when they are most actionable.
Clinical decision support should be evidence-based, regularly updated, and tuned to minimize alert fatigue while highlighting truly significant issues. Support can range from passive information display to interruptive alerts for critical safety issues. User feedback should inform ongoing refinement of decision support rules, ensuring they remain clinically relevant and appropriately sensitive.
Privacy and Consent Management
Beyond technical security controls, organizations must establish policies and processes for managing patient privacy preferences and consent. Patients should have transparency into who is accessing their information and for what purposes. Break-the-glass procedures allow emergency access to records when patient safety requires it, even when normal access controls would prevent it, while logging such access for subsequent review.
Consent management capabilities enable patients to grant or restrict access to specific information or by specific providers. This is particularly important for sensitive services like behavioral health, substance abuse treatment, or reproductive health, where patients may wish to maintain additional privacy. Organizations must balance patient privacy preferences with care coordination needs, developing policies that respect patient autonomy while ensuring providers have information necessary for safe, effective care.
Advanced Features and Emerging Capabilities
Remote Patient Monitoring Integration
The integration of remote patient monitoring (RPM) devices and data streams into the 360-degree patient view represents a significant advancement in care delivery. Patients with chronic conditions can use connected devices to measure vital signs, blood glucose, weight, activity levels, and other health parameters in their homes. This data flows into Health Cloud, where it is displayed alongside other clinical information and analyzed for concerning trends.
Automated alerts notify care teams when monitored values fall outside acceptable ranges, enabling proactive intervention before situations escalate to emergency department visits or hospitalizations. Care protocols can be configured to trigger specific workflows based on RPM data—for example, a care coordinator might call a heart failure patient whose weight has increased significantly over several days, indicating fluid retention. This early intervention can prevent decompensation and hospitalization while providing patients with support and reassurance in their home environment.
Social Collaboration and Care Team Communication
Effective care coordination requires seamless communication among multidisciplinary care team members. Health Cloud incorporates social collaboration features similar to enterprise social networks, allowing team members to communicate about specific patients, share information, and coordinate activities. Care team channels for individual patients or patient cohorts enable secure, HIPAA-compliant collaboration without relying on insecure communication methods like personal email or text messaging.
@mentions allow users to tag specific team members who need to be aware of information or take action. File sharing enables distribution of relevant documents, images, or resources within the care team. Activity feeds provide a chronological view of care team communications and activities, creating transparency and ensuring all team members remain informed about patient status and care plan execution.
Mobile Access and Field Workforce Support
Healthcare delivery increasingly occurs outside traditional clinical settings, with home health nurses, community health workers, and mobile care teams providing services in patients’ homes and communities. Mobile-optimized interfaces provide field workers with access to the 360-degree patient view on smartphones and tablets, ensuring they have necessary patient information regardless of location.
Offline capabilities allow continued access to patient data and documentation even when internet connectivity is unavailable. Changes made while offline are synchronized when connectivity is restored, ensuring information flows back to central systems. GPS integration can provide location-based features like optimized routing for home visits or identification of patients living in specific geographic areas for community-based interventions.
Precision Medicine and Genomics Integration
As precision medicine becomes more mainstream, the 360-degree patient view is evolving to incorporate genomic data, genetic test results, and pharmacogenomic information that informs medication selection and dosing. Genetic variants associated with disease risk, drug metabolism, and treatment response can be displayed alongside traditional clinical information, enabling more personalized treatment recommendations.
Decision support systems can leverage genomic information to recommend medications less likely to cause adverse reactions or more likely to be effective based on patient genetics. Family history analysis combined with genetic data enables more accurate risk assessment for hereditary conditions. As genomic testing becomes more affordable and prevalent, this integration will become increasingly important for delivering truly personalized healthcare.
Measuring Success and Continuous Improvement
Key Performance Indicators
Organizations should establish clear metrics for evaluating the impact of their 360-degree patient view implementation. Clinical outcome metrics might include hospital readmission rates, emergency department utilization, disease control measures, or preventable complication rates. Operational metrics could track care team efficiency, documentation completeness, or time spent searching for patient information. Patient experience measures including satisfaction scores, patient activation levels, and engagement rates provide patient-centered perspectives on value.
Financial metrics relevant to value-based contracts, total cost of care, or revenue cycle performance demonstrate the business case for comprehensive patient views. Quality measure performance on payer or regulatory reporting requirements shows impact on organizational priorities. User satisfaction surveys and system utilization rates indicate whether care teams are adopting and finding value in the platform.
Continuous Optimization
Health Cloud implementations should be viewed as ongoing programs rather than one-time projects. Regular review of usage patterns, user feedback, and performance metrics identifies opportunities for refinement and enhancement. Configuration changes might optimize workflows, add new data sources, or incorporate new decision support rules based on emerging clinical evidence.
User communities and advisory groups provide structured mechanisms for gathering input from frontline users. Quarterly or annual release cycles introduce new capabilities, address identified issues, and keep the platform aligned with evolving organizational needs. Benchmarking against other organizations using Health Cloud can identify best practices and innovative use cases to consider adopting.
Conclusion
The 360-degree patient view in Salesforce Health Cloud represents a paradigm shift in how healthcare information is organized, accessed, and utilized to improve care delivery. By consolidating fragmented data into comprehensive, actionable patient profiles, the platform enables care teams to deliver more coordinated, personalized, and effective care. The technical foundation built on industry standards ensures interoperability with existing healthcare IT infrastructure while maintaining the highest levels of security and privacy protection.
Success with Health Cloud requires more than technology implementation—it demands attention to data quality, change management, workflow integration, and ongoing optimization. Organizations that approach implementation strategically, with clear goals and sustained commitment, can achieve significant improvements in clinical outcomes, operational efficiency, patient experience, and financial performance.
As healthcare continues its evolution toward value-based models, population health management, and patient-centered care, comprehensive patient views will become increasingly essential infrastructure. Salesforce Health Cloud provides a mature, flexible platform that can grow with organizations as their needs evolve, supporting current requirements while enabling future innovation in care delivery models and health information technology.
The future of healthcare depends on breaking down information silos, enabling seamless collaboration among care teams, engaging patients as active participants in their care, and leveraging data and analytics to drive continuous improvement. The 360-degree patient view in Salesforce Health Cloud provides the foundation for this future, empowering healthcare organizations to deliver the right care, to the right patient, at the right time, every time.
About RizeX Labs
At RizeX Labs, we specialize in delivering advanced healthcare solutions powered by Salesforce Health Cloud. Our expertise combines deep technical knowledge, healthcare industry best practices, and real-world implementation experience to help organizations improve patient care, streamline operations, and ensure compliance.
We empower healthcare providers, payers, and life sciences organizations to transform fragmented systems into unified, intelligent care platforms—enabling personalized patient engagement, coordinated care, and better health outcomes.
Internal Linking Opportunities:
- Link to your Salesforce course page:
https://rizexlabs.com/salesforce-admin-and-development-training
External Linking Opportunities:
- Salesforce official website: https://www.salesforce.com/
- Salesforce Health Cloud overview: https://www.salesforce.com/products/health-cloud/overview/
- Salesforce documentation: https://help.salesforce.com/
- Salesforce AppExchange: https://appexchange.salesforce.com/
- Healthcare interoperability standard (FHIR): https://www.hl7.org/fhir/
- HIPAA compliance guidelines: https://www.hhs.gov/hipaa/index.html
- MuleSoft (for healthcare integrations): https://www.mulesoft.com/
Quick Summary
Salesforce Health Cloud is a powerful healthcare CRM platform designed to provide a 360-degree view of patients, enabling organizations to deliver personalized, connected, and proactive care. It integrates clinical and non-clinical data from multiple systems, helping care teams make informed decisions faster.
With Health Cloud, healthcare organizations can improve patient engagement, enhance care coordination, ensure regulatory compliance, and reduce operational inefficiencies. As the healthcare ecosystem becomes more data-driven, adopting Health Cloud is essential for delivering modern, patient-centric care at scale.
Quick Summary
The Salesforce Health Cloud 360-degree patient view is a system that consolidates fragmented healthcare data—such as medical history, medications, clinical visits, diagnostics, care teams, insurance details, and social factors—into a single unified dashboard, enabling healthcare providers to access a complete and real-time picture of a patient’s health journey. Built on interoperability standards like FHIR and enhanced with AI-driven insights, it supports better decision-making, care coordination, chronic disease management, and patient engagement while ensuring data security and compliance. However, its success heavily depends on high-quality data, proper integration with existing systems, and effective user adoption, making it not just a technology solution but a comprehensive transformation in healthcare data management and delivery.


