Introduction: The Hidden Environmental Cost of Healthcare IT
Healthcare facilities consume approximately 10% of all commercial building energy in the United States, with data centers and IT infrastructure accounting for an increasingly significant portion of that consumption. A typical 400-bed hospital generates roughly 30 pounds of waste per bed per day and consumes energy equivalent to a small city—much of it driven by outdated, on-premises IT systems running 24/7 to support critical patient care operations.

The irony is stark: an industry dedicated to human health is simultaneously contributing to environmental degradation that undermines public health outcomes. Traditional hospital data centers require massive cooling systems, redundant power supplies, and constant energy consumption regardless of actual computing demand. As healthcare organizations digitize patient records, deploy AI-powered diagnostics, and implement remote monitoring systems, their IT infrastructure’s carbon footprint continues to grow exponentially.
Green Cloud in Healthcare represents a strategic approach to delivering IT services through sustainable cloud infrastructure that dramatically reduces energy consumption, carbon emissions, and environmental waste while improving operational efficiency. For healthcare IT leaders facing pressure to meet sustainability goals without compromising patient care or security, cloud migration offers a concrete pathway to measurable environmental impact.
This article examines how healthcare organizations can leverage green cloud technologies to reduce their carbon footprint while achieving superior business outcomes—from cost reduction to enhanced scalability and regulatory compliance.
Understanding Green Cloud in Healthcare Context
What Makes Cloud Infrastructure “Green”
Green Cloud in Healthcare refers to cloud computing services delivered through data centers optimized for energy efficiency and powered by renewable energy sources. Unlike traditional definitions of cloud computing that focus solely on virtualization and on-demand resources, green cloud emphasizes environmental sustainability as a core architectural principle.
Major cloud providers have made substantial commitments to sustainability:
- Google Cloud has been carbon-neutral since 2007 and achieved 100% renewable energy matching for global operations since 2017, with a commitment to operate on 24/7 carbon-free energy by 2030
- Microsoft Azure achieved carbon neutrality in 2012 and committed to being carbon negative by 2030, with plans to remove all historical carbon emissions by 2050
- AWS committed to powering operations with 100% renewable energy by 2025 (five years ahead of the original 2030 target) and achieving net-zero carbon by 2040
These hyperscale cloud providers achieve energy efficiency that individual hospital data centers cannot match through several mechanisms:
Advanced cooling technologies: Liquid cooling, free air cooling, and AI-optimized thermal management systems reduce cooling energy by 30-40% compared to traditional approaches.
Power Usage Effectiveness (PUE): Leading cloud data centers achieve PUE ratings between 1.1 and 1.2, meaning only 10-20% overhead energy consumption beyond computing. Traditional enterprise data centers typically operate at PUE of 1.8-2.0, consuming 80-100% additional energy for cooling and power distribution.
Resource utilization optimization: Through multi-tenancy and dynamic resource allocation, cloud infrastructure maintains server utilization rates of 65-75%, compared to 15-20% in typical on-premises healthcare data centers.
Renewable energy procurement: Hyperscale providers negotiate power purchase agreements for wind and solar at volumes impossible for individual healthcare organizations.
The Healthcare-Specific Sustainability Challenge
Healthcare organizations face unique constraints that make green cloud adoption both more challenging and more necessary:
Always-on requirements: Electronic health records (EHR), patient monitoring systems, and emergency department operations require 99.99% uptime, creating pressure to over-provision infrastructure.
Data sovereignty and compliance: HIPAA, HITECH, and state-level privacy regulations create complexity around data residency that can limit cloud region selection.
Legacy system integration: Many hospitals operate core systems 15-20 years old that weren’t designed for cloud environments.
Budget constraints: Healthcare operates on notoriously thin margins (2-4% for many systems), making large IT infrastructure investments difficult to justify despite long-term savings.
Despite these challenges, healthcare organizations that successfully implement green cloud strategies typically achieve 65-85% reduction in IT-related carbon emissions while realizing 30-40% cost savings over three to five years.
Key Challenges in Traditional Hospital IT Infrastructure
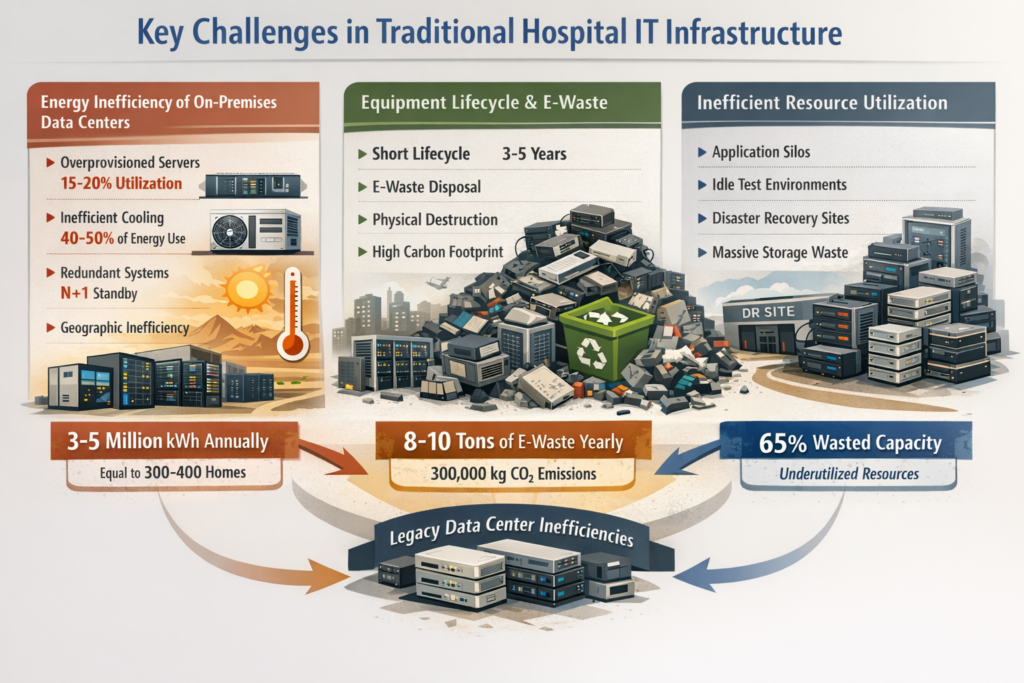
Energy Inefficiency of On-Premises Data Centers
Traditional hospital data centers were designed during an era when computational needs were more predictable and energy costs represented a smaller portion of operational budgets. These legacy environments create multiple inefficiency layers:
Overprovisioning for peak demand: Hospitals provision infrastructure to handle peak loads that occur only 5-10% of the time. During normal operations, servers run at 15-20% capacity while consuming 60-70% of peak power due to static power consumption characteristics.
Inefficient cooling requirements: A 200-rack hospital data center typically requires 200-300 tons of cooling capacity running continuously. Older facilities use computer room air conditioning (CRAC) units with efficiency ratios significantly worse than modern cooling approaches. The cooling infrastructure alone can consume 40-50% of total data center energy.
Redundancy waste: Healthcare’s uptime requirements lead to N+1 or 2N redundancy configurations where backup systems sit idle but fully powered. While redundancy is essential for patient safety, traditional approaches waste enormous energy maintaining redundant infrastructure at full operational power.
Geographic inefficiency: Hospital data centers operate in locations chosen for clinical proximity rather than energy efficiency. A data center in Phoenix runs dramatically different cooling costs than one in Seattle, yet hospitals have historically made no distinction.
A typical 400-bed hospital operating its own data center consumes approximately 3-5 million kWh annually just for IT infrastructure—equivalent to the energy consumption of 300-400 average American homes.
Equipment Lifecycle and E-Waste
Healthcare IT infrastructure generates substantial electronic waste through accelerated replacement cycles:
Short useful life: Servers, storage arrays, and networking equipment typically operate for 3-5 years before requiring replacement due to warranty expiration, capacity limitations, or vendor support discontinuation.
Disposal challenges: Healthcare organizations must ensure data sanitization before disposal, leading many to physically destroy storage devices rather than refurbish them. This approach maximizes waste while minimizing equipment reuse.
Embodied carbon: Manufacturing a single server produces approximately 1,200-2,000 kg of CO2 equivalent emissions before it ever processes a single transaction. Frequent replacement cycles multiply this manufacturing carbon footprint.
Component-level waste: When a storage array reaches capacity limits, hospitals often replace the entire system rather than expanding capacity, discarding functioning components with significant remaining useful life.
A mid-size hospital system refreshing 200 servers on a four-year cycle generates approximately 8-10 tons of e-waste annually, representing roughly 300,000 kg of embodied carbon in new equipment manufacturing.
Inefficient Resource Utilization
Traditional infrastructure architectures create structural resource waste:
Application silos: Healthcare applications often run on dedicated physical servers due to vendor requirements or internal risk management policies. This one-application-per-server model wastes enormous capacity. A single EHR production server might consume 8-12% average CPU while reserving an entire physical machine.
Development and testing environments: Hospitals maintain separate development, testing, and training environments that mirror production infrastructure. These environments sit idle 60-70% of the time while consuming nearly full power.
Disaster recovery infrastructure: DR sites maintain near-complete infrastructure replicas that process zero production workload until disaster strikes. This represents a necessary business continuity investment but one that consumes continuous energy for intermittent value.
Storage inefficiency: Healthcare data has strict retention requirements (often 7-10 years for adult records, longer for pediatric), leading to massive storage infrastructure supporting infrequently accessed data. Traditional storage architectures apply the same performance (and power consumption) characteristics to all data regardless of access frequency.
Research indicates that the average hospital data center wastes approximately 65% of provisioned capacity through these structural inefficiencies—capacity that nonetheless consumes power, cooling, and space continuously.
How Cloud Infrastructure Reduces Healthcare’s Carbon Footprint
Energy Efficiency Through Hyperscale Operations
Cloud providers achieve energy efficiency impossible for individual healthcare organizations through operational scale and specialized expertise:
Optimized power distribution: Hyperscale data centers use high-voltage DC power distribution and custom power supplies that reduce conversion losses from 15-20% down to 5-8%. At scale, this represents enormous energy savings.
Advanced thermal management: Cloud providers employ computational fluid dynamics modeling to optimize airflow, AI-driven cooling adjustments that respond to actual thermal loads in real-time, and free cooling techniques that use outside air when ambient conditions allow.
Google’s data centers, for example, use DeepMind AI to predict thermal loads and optimize cooling 40% more effectively than human operators, reducing overall energy consumption for cooling by 30%.
Server efficiency: Cloud providers use custom-designed servers optimized for specific workloads. AWS Graviton processors, for instance, provide up to 60% better performance per watt than comparable x86 processors for many workloads.
Location optimization: Cloud providers strategically locate data centers in regions with favorable climates for cooling and access to renewable energy. Microsoft’s data centers in Finland use seawater cooling, while AWS facilities in Oregon access abundant hydroelectric power.
Dynamic resource allocation: Cloud infrastructure automatically scales resources to match actual demand. During low-utilization periods (nights, weekends), the platform reduces active servers and consolidates workloads, reducing power consumption proportionally. Healthcare workloads with predictable patterns (like monthly billing or analytical workloads) can leverage this elasticity for substantial efficiency gains.
For healthcare organizations, migrating to hyperscale cloud infrastructure typically reduces per-workload energy consumption by 65-80% compared to on-premises operations.
Renewable Energy Integration
Cloud providers’ renewable energy commitments deliver immediate carbon reduction benefits to healthcare customers:
Power Purchase Agreements (PPAs): Major cloud providers are among the world’s largest corporate purchasers of renewable energy. In 2022 alone, AWS, Azure, and Google Cloud collectively purchased over 30 gigawatts of renewable energy capacity. Individual healthcare systems cannot negotiate PPAs at this scale.
Renewable Energy Certificates (RECs): Cloud providers match energy consumption with renewable energy generation through RECs, effectively ensuring that for every megawatt-hour consumed, a megawatt-hour of renewable energy is added to the grid.
24/7 carbon-free energy matching: Google Cloud offers region selection based on carbon-free energy percentage, allowing healthcare organizations to choose data center locations with the highest renewable energy mix. Some regions exceed 90% carbon-free energy on a time-matched basis.
Transparency and reporting: Cloud providers offer carbon footprint reporting tools that help healthcare organizations measure and report Scope 3 emissions from IT operations. AWS Customer Carbon Footprint Tool, Azure Carbon Optimization, and Google Cloud Carbon Footprint provide detailed emissions data mapped to specific workloads.
A 250-bed hospital migrating its EHR and associated applications to a cloud region powered by 80% renewable energy can reduce IT-related carbon emissions by approximately 200-250 metric tons of CO2 equivalent annually—equivalent to removing 45-50 cars from the road.
Improved Resource Utilization and Right-Sizing
Cloud infrastructure’s on-demand model fundamentally changes resource economics:
Workload-appropriate sizing: Rather than provisioning for peak load, healthcare organizations can dynamically scale resources to match actual demand. An imaging processing workload that runs nightly can scale up for 4-6 hours and scale down to minimal resources during the day.
Environment efficiency: Development, testing, and training environments can be shut down outside business hours or created on-demand for specific testing cycles. A test environment that runs 40 hours per week instead of 168 hours reduces energy consumption by 76%.
Serverless architectures: For event-driven workloads (like HL7 message processing, notification systems, or data transformations), serverless computing eliminates idle resource consumption entirely. Resources exist only during execution, potentially reducing energy consumption by 90%+ for appropriate workloads.
Automated optimization: Cloud platforms provide recommendations for right-sizing resources based on actual utilization patterns. Azure Advisor, AWS Compute Optimizer, and Google Cloud Recommender identify over-provisioned resources and suggest more efficient configurations.
Storage tiering: Cloud providers offer multiple storage tiers with different performance and power characteristics. Frequently accessed data lives on high-performance storage, while archived medical records move to cold storage that consumes 90% less energy. Automated lifecycle policies move data between tiers without manual intervention.
Cleveland Clinic reported 40% improvement in resource utilization after migrating development and test environments to Azure, eliminating approximately 150 metric tons of annual CO2 emissions while reducing infrastructure costs by $2.3 million annually.
Extended Hardware Lifecycles and Reduced E-Waste
Cloud migration fundamentally changes healthcare organizations’ relationship with hardware:
Elimination of on-premises refresh cycles: Healthcare organizations no longer purchase, deploy, and dispose of servers on 3-5 year cycles. Cloud providers manage hardware lifecycles at massive scale with sophisticated reuse and recycling programs.
Component reuse: When cloud providers decommission servers, they harvest functional components for reuse, remanufacture equipment for secondary markets, or recycle materials through specialized e-waste programs. Microsoft’s Circular Centers recover and reuse 90% of server components.
Extended useful life: Cloud providers operate servers longer than typical enterprise refresh cycles by continuously upgrading components, optimizing workload placement for aging hardware, and maintaining older equipment for appropriate workload types.
Reduced endpoint hardware: Virtual desktop infrastructure (VDI) and cloud-based applications reduce requirements for powerful endpoint devices. Clinicians can access EHR systems from tablets, thin clients, or repurposed older PCs rather than requiring new workstations every 3-4 years.
A 300-bed hospital eliminating a 150-server on-premises data center avoids approximately 180 metric tons of embodied carbon over a five-year period while reducing e-waste by 22-25 tons.
Real-World Healthcare Use Cases and Results
Case Study: Partners HealthCare System (Mass General Brigham)
Partners HealthCare (now Mass General Brigham), one of America’s largest healthcare systems with 12 hospitals and 6,900+ physicians, undertook a major cloud migration initiative focused on sustainability and operational efficiency.
Challenge: The organization operated seven on-premises data centers with approximately 14,000 physical servers consuming roughly 42 million kWh annually. Aging infrastructure required significant capital investment for refresh cycles.
Approach: Phased migration to AWS focusing initially on non-production environments, followed by analytics workloads, administrative systems, and select clinical applications. The organization implemented cloud center of excellence practices to optimize resource utilization from inception.
Results:
- 65% reduction in IT infrastructure energy consumption
- Approximately 21,000 metric tons of CO2 equivalent emissions reduction annually
- $35 million in avoided capital expenditure over five years
- 40% reduction in IT infrastructure operating costs
- Improved disaster recovery capabilities with testing conducted quarterly rather than annually
Key sustainability factors:
- Migrated workloads to AWS US-East-1 (Virginia) region where AWS achieved 95% renewable energy matching
- Implemented auto-scaling for development/test environments, reducing runtime by 60%
- Adopted serverless architectures for data processing pipelines, reducing compute hours by 45%
- Used S3 Intelligent-Tiering for medical imaging archives, reducing storage-related energy consumption by 70%
Case Study: Advocate Aurora Health
Advocate Aurora Health, a 27-hospital system serving communities in Illinois and Wisconsin, focused its cloud strategy explicitly on sustainability alignment with organizational environmental goals.
Challenge: The health system committed to reducing carbon emissions by 50% by 2030. IT infrastructure represented approximately 12% of total organizational emissions, creating an opportunity for measurable impact.
Approach: Hybrid cloud architecture with Microsoft Azure as primary cloud platform, maintaining critical on-premises systems while migrating analytics, collaboration tools, population health platforms, and administrative applications to cloud.
Results:
- 8,400 metric tons of CO2 equivalent emissions reduction in first 18 months
- 38% reduction in IT energy consumption
- $4.2 million annual cost savings from reduced data center operations
- 50% faster deployment of new analytical capabilities
- Improved staff productivity through Office 365 migration
Key sustainability factors:
- Selected Azure regions (US North Central and US East) with high renewable energy percentages
- Implemented Azure Virtual Desktop to extend life of 3,500 endpoint devices by 2+ years
- Used Azure Blob Storage cool and archive tiers for long-term medical record retention
- Deployed Azure sustainability calculator to measure and report emissions reduction quarterly
- Integrated cloud carbon footprint into IT project approval process
Case Study: UC San Diego Health
UC San Diego Health implemented a research-focused cloud strategy that addressed both operational systems and research computing’s substantial energy footprint.
Challenge: Research computing for genomics, medical imaging research, and clinical trials consumed enormous computational resources with highly variable demand. Traditional infrastructure remained underutilized 70% of the time but couldn’t scale for peak research needs.
Approach: Hybrid architecture with Google Cloud Platform for research computing and select operational workloads while maintaining Epic EHR on-premises with cloud disaster recovery.
Results:
- 72% reduction in research computing energy consumption
- 4,800 metric tons of CO2 equivalent annual emissions reduction
- 400% improvement in research computational capacity during peak periods
- 35% reduction in IT infrastructure costs
- Accelerated research timelines through burst computing capabilities
Key sustainability factors:
- Leveraged Google Cloud’s Iowa and Oregon regions with high renewable energy percentages
- Implemented preemptible instances for fault-tolerant research workloads, reducing costs by 70% and prioritizing workload efficiency
- Used BigQuery for large-scale research data analytics instead of maintaining dedicated analytics infrastructure
- Deployed Cloud Functions for data processing pipelines, eliminating idle compute resources
- Established sustainability metrics as part of research computing resource allocation decisions
Medical Imaging Archiving and Communication Systems (PACS)
Medical imaging represents one of healthcare’s most significant and fastest-growing IT infrastructure challenges. A typical 400-bed hospital with comprehensive imaging services generates 20-40 terabytes of new imaging data annually, with 7-10 year retention requirements creating an ever-expanding storage footprint.
Traditional approach challenges:
- On-premises PACS storage systems consume substantial power for cooling and disk operation
- High-performance storage maintains all images with identical access characteristics despite 80% of images being accessed only within the first 90 days
- Geographic redundancy requires duplicate infrastructure and power consumption
Cloud-based PACS benefits:
Storage tiering optimization: Cloud providers offer multiple storage tiers with dramatically different energy profiles. Recent studies (< 90 days) remain in high-performance storage, while older studies migrate automatically to cold storage consuming 90% less energy.
Intelligent prefetching: Machine learning algorithms predict which historical studies clinicians will likely access based on patient encounters, pre-loading relevant images to high-performance tiers.
Vendor-neutral archives: Cloud-based VNAs consolidate imaging from multiple PACS systems, eliminating redundant storage and enabling more efficient lifecycle management.
Results from implementations:
- Sentara Healthcare reduced imaging storage energy consumption by 68% after migrating to AWS S3 with intelligent tiering
- Intermountain Healthcare achieved 55% cost reduction for imaging storage while improving disaster recovery capabilities
- Memorial Hermann Health System reported 40% reduction in PACS-related energy consumption after Azure migration
Remote Patient Monitoring and IoT Applications
Healthcare Internet of Things (IoT) applications—including remote patient monitoring, asset tracking, and environmental monitoring—generate substantial data requiring processing and storage infrastructure.
Cloud advantages for healthcare IoT:
Edge computing integration: Azure IoT Edge and AWS IoT Greengrass enable local processing that reduces data transmission and centralized processing requirements. Only medically significant events or aggregated data transmit to cloud, reducing network energy consumption and cloud processing requirements.
Serverless data processing: Event-driven architectures process IoT data only when it arrives, eliminating continuously running processing infrastructure. For monitoring 1,000 patients generating intermittent vital signs data, serverless approaches reduce processing energy consumption by 85-90% compared to continuously running servers.
Intelligent data retention: Most IoT data has declining value over time. Automated policies retain high-frequency data for acute periods (24-72 hours), then downsample and archive, reducing long-term storage footprint by 95%+.
Results from implementations:
- Kaiser Permanente’s remote monitoring program supporting 50,000+ patients uses Azure IoT with reported 40% lower infrastructure costs and 60% reduced energy consumption compared to on-premises alternatives
- VA health system’s asset tracking implementation eliminated 12 on-premises servers, reducing energy consumption by 85 metric tons of CO2 equivalent annually
Business Benefits Beyond Sustainability
While environmental impact drives initial interest in Green Cloud in Healthcare, business benefits often provide the ultimate justification for migration projects.

Cost Reduction and Financial Performance
Cloud migration delivers quantifiable financial benefits that improve healthcare organizations’ operating margins:
Capital expenditure elimination: Cloud shifts IT infrastructure from capital to operational expenditure, eliminating large upfront investments. A 300-bed hospital can avoid $3-5 million in server, storage, and network equipment purchases over a five-year period.
Reduced facilities costs: Smaller or eliminated data centers reduce power consumption, cooling costs, and facility space requirements. The space reclaimed from data center decommissioning can be repurposed for revenue-generating clinical use. A mid-size hospital typically saves $400,000-$800,000 annually in data center facilities costs.
Operational efficiency: Cloud platforms reduce staffing requirements for infrastructure management. While cloud introduces new skill requirements, organizations typically reduce low-level infrastructure management tasks (hardware maintenance, OS patching, capacity planning) by 60-70%, allowing IT staff to focus on higher-value activities.
Predictable costs: Reserved instances and savings plans provide predictable pricing for steady-state workloads, while on-demand pricing for variable workloads eliminates overprovisioning costs. Organizations typically reduce infrastructure costs by 30-40% compared to on-premises equivalents.
Energy cost reduction: A 400-bed hospital eliminating an on-premises data center reduces annual electricity costs by $400,000-$700,000 depending on local energy rates.
Financial results: Providence St. Joseph Health reported $150 million in cost savings over five years from cloud migration, with 35% attributed directly to infrastructure cost reduction and energy efficiency.
Operational Resilience and Business Continuity
Healthcare organizations face unique operational continuity requirements where downtime directly impacts patient safety:
Geographic redundancy: Cloud providers offer multi-region deployment with automated failover at costs impossible for individual organizations. A hospital can maintain active-active EHR deployment across multiple geographic regions for lower cost than traditional single-site disaster recovery.
Rapid disaster recovery: Cloud-based backup and disaster recovery solutions reduce recovery time objectives (RTOs) from hours to minutes. During Hurricane Harvey, Memorial Hermann Health System maintained operations using Azure-based disaster recovery despite primary data center flooding.
Reduced testing complexity: Cloud environments enable realistic disaster recovery testing without complex on-premises coordination. Organizations can test quarterly or monthly rather than annually, improving confidence in recovery procedures.
Automated backup and retention: Cloud platforms provide automated backup with immutable storage options that protect against ransomware. Version control and point-in-time recovery capabilities exceed traditional backup systems.
Results: Hospitals implementing cloud-based disaster recovery report 75-85% reduction in DR infrastructure costs while improving RTOs by 90% and reducing data loss potential by 95%.
Scalability and Innovation Acceleration
Cloud infrastructure removes traditional constraints on innovation and growth:
Rapid environment provisioning: New applications, testing environments, or analytical workloads deploy in minutes rather than weeks or months required for on-premises infrastructure procurement and deployment.
Elastic capacity: Healthcare organizations can handle unpredictable demand spikes (pandemic response, seasonal flu, unexpected patient surges) without permanently provisioning for peak capacity.
Advanced technology access: Cloud providers invest billions in artificial intelligence, machine learning, and analytical capabilities. Healthcare organizations access these technologies on consumption-based pricing rather than requiring million-dollar infrastructure investments.
Multi-site deployment: Health systems with multiple hospitals can standardize infrastructure across facilities and deploy new capabilities simultaneously rather than sequential rollouts limited by infrastructure capacity.
Innovation examples:
- UPMC deployed COVID-19 screening and vaccination management applications in 72 hours using AWS serverless architecture—a timeline impossible with traditional infrastructure
- Johns Hopkins researchers reduced genomic sequencing analysis time from weeks to hours using Google Cloud’s AI and computing capabilities
- Cleveland Clinic deployed AI-powered sepsis prediction across all facilities within 30 days using Azure Machine Learning
Regulatory Compliance and Security
Cloud platforms provide security and compliance capabilities that exceed most healthcare organizations’ on-premises environments:
HIPAA compliance infrastructure: All major cloud providers offer HIPAA-eligible services with Business Associate Agreements (BAAs), maintaining compliance certifications that individual organizations would spend millions to achieve.
Security at scale: Cloud providers employ thousands of security professionals and invest billions in security infrastructure. They detect and respond to threats faster than individual organizations and implement security patches at scale.
Compliance certifications: Cloud platforms maintain certifications for HITRUST, SOC 2, ISO 27001, and other healthcare-relevant frameworks, reducing compliance burden for customers.
Audit and monitoring: Built-in logging, monitoring, and threat detection capabilities provide visibility that requires significant investment to replicate on-premises. Cloud platforms detect anomalous behavior patterns across millions of customers, identifying threats before they impact individual organizations.
Data sovereignty controls: Cloud regions and availability zones enable precise control over data location to meet state-level privacy requirements and data residency regulations.
Results: Healthcare organizations report 40-60% reduction in security incident frequency after cloud migration, with faster detection and remediation of incidents that do occur.
Implementation Challenges and Practical Limitations
Despite substantial benefits, Green Cloud in Healthcare implementation faces real challenges that organizations must address:
Application Compatibility and Vendor Constraints
Healthcare organizations operate complex application portfolios with varying cloud readiness:
Legacy clinical applications: Many core clinical systems were designed for on-premises deployment decades ago. Epic, Cerner (now Oracle Health), and Meditech have historically optimized for on-premises deployment, though cloud options are evolving.
Vendor support limitations: Some healthcare software vendors don’t support cloud deployments or charge substantial premiums for cloud-based licensing. Vendors may restrict which cloud providers or regions customers can use.
Integration complexity: Healthcare organizations operate 200-300+ applications with complex integration requirements. Point-to-point integrations designed for on-premises deployment may require redesign for cloud environments.
Performance concerns: Some imaging applications and real-time monitoring systems have latency requirements that complicate cloud deployment. Organizations must carefully evaluate network latency impacts on user experience.
Mitigation approaches:
- Start with cloud-ready applications (collaboration tools, analytics, administrative systems) before tackling complex clinical applications
- Work with vendors on cloud deployment roadmaps and include cloud support in procurement requirements
- Consider hybrid architectures that keep latency-sensitive applications on-premises while moving supporting systems to cloud
- Implement cloud-based disaster recovery for on-premises systems as an intermediate step
Data Migration Complexity and Risk
Moving protected health information to cloud involves substantial planning and risk management:
Data volume challenges: Healthcare organizations store petabytes of data. A large health system might need to migrate 10-20 petabytes of imaging, EMR data, and administrative information. At typical network speeds, this could take months.
Downtime constraints: Core clinical systems operate 24/7 with minimal tolerance for downtime. Migration windows must be carefully planned and validated through extensive testing.
Data validation requirements: Healthcare organizations must validate data integrity post-migration with sampling approaches that balance thoroughness against timeline pressures.
Compliance during migration: PHI must remain protected throughout migration. Encryption in transit and at rest, access controls, and audit logging must function throughout the migration process.
Cost of migration: Data egress from on-premises to cloud, migration tools, consulting services, and increased staffing during migration create substantial costs that must be factored into business cases.
Mitigation approaches:
- Use AWS DataSync, Azure Data Box, or Google Transfer Appliance for large datasets to avoid network bandwidth limitations
- Implement phased migrations starting with non-production data to validate processes before production migration
- Maintain parallel environments during cutover periods to enable rollback if issues arise
- Use cloud provider migration services and experienced consulting partners for complex migrations
Skills Gap and Organizational Change
Cloud adoption requires new skills and organizational changes that many healthcare IT teams struggle with:
Infrastructure-as-code approaches: Cloud environments managed through code (Terraform, CloudFormation, ARM templates) require different skills than GUI-based on-premises management.
Security model differences: Shared responsibility model requires healthcare organizations to understand where provider responsibility ends and customer responsibility begins. Misunderstanding this division creates security vulnerabilities.
Cost management complexity: Unlike fixed infrastructure costs, cloud consumption-based pricing creates cost management challenges. Without proper governance, cloud costs can exceed on-premises equivalents.
Operational model changes: Cloud platforms update continuously with new features and deprecations. Organizations must establish processes for evaluating and adopting changes rather than maintaining static environments.
Cultural resistance: IT staff may resist cloud adoption due to concerns about job security or preference for familiar technologies. Clinical and administrative users may resist changes to workflows or application interfaces.
Mitigation approaches:
- Invest in cloud training and certification for IT staff (AWS Certified Solutions Architect, Azure Administrator, Google Cloud Professional Architect)
- Hire cloud-experienced staff for key leadership positions
- Establish cloud center of excellence to develop standards, governance, and shared knowledge
- Implement FinOps practices for cloud cost management with accountability at application/department level
- Communicate early and often about cloud strategy, timelines, and expected changes
Network Dependency and Connectivity Requirements
Cloud-based applications create new dependencies on network connectivity:
Internet dependency: Cloud services require reliable internet connectivity. Network outages that previously impacted email might now affect clinical applications.
Bandwidth requirements: Imaging applications, VDI, and real-time monitoring require substantial bandwidth. Organizations must upgrade internet connectivity—often requiring 5-10x bandwidth increases.
Latency considerations: Round-trip network latency to cloud services impacts application responsiveness. A 50-100ms latency that’s imperceptible for web browsing may degrade clinical application user experience.
Cost of connectivity: High-bandwidth, low-latency connectivity is expensive. Organizations may spend $50,000-$200,000+ monthly on internet connectivity and direct cloud connections.
Rural and remote challenges: Smaller hospitals in rural areas may lack access to high-speed, redundant internet connectivity, limiting cloud application options.
Mitigation approaches:
- Implement redundant internet connections from diverse providers with automated failover
- Use AWS Direct Connect, Azure ExpressRoute, or Google Cloud Interconnect for predictable, high-bandwidth connectivity
- Deploy edge caching and local processing for latency-sensitive applications
- Maintain limited on-premises infrastructure for break-glass scenarios during network outages
- Consider hybrid architectures for organizations with connectivity constraints
Best Practices for Green Cloud Implementation in Healthcare
Start with Sustainability Measurement and Goals
Successful green cloud initiatives begin with baseline measurement and clear objectives:
Conduct carbon footprint assessment: Measure current IT infrastructure energy consumption and associated carbon emissions. This requires:
- Complete inventory of servers, storage, networking equipment with power consumption specifications
- Data center power and cooling measurements
- Electricity carbon intensity for facility locations (varies significantly by region based on grid energy sources)
- Manufacturing embodied carbon for planned equipment refresh cycles
Establish measurable targets: Set specific, time-bound sustainability goals aligned with organizational environmental commitments. Examples include:
- Reduce IT-related carbon emissions by 50% within three years
- Achieve 80% renewable energy for IT infrastructure within 24 months
- Reduce IT e-waste by 75% over five years
Create measurement framework: Implement tools and processes to track progress:
- Use cloud provider carbon footprint tools (AWS Customer Carbon Footprint Tool, Azure Carbon Optimization, Google Cloud Carbon Footprint)
- Establish quarterly reporting on key metrics (energy consumption, carbon emissions, renewable energy percentage)
- Include sustainability metrics in IT project evaluation criteria
- Report IT sustainability performance to board and executive leadership
Practice example: Before starting its cloud migration, Stanford Health Care conducted detailed assessment identifying that IT infrastructure generated 18,500 metric tons of CO2 equivalent annually. They established a goal of 60% reduction within three years, with quarterly tracking and public reporting.
Adopt Cloud-Native Architectures
Maximizing green cloud benefits requires architectural approaches that leverage cloud characteristics:
Microservices and serverless: Break monolithic applications into smaller services that scale independently. Use serverless computing (AWS Lambda, Azure Functions, Google Cloud Functions) for event-driven workloads to eliminate idle resource consumption.
Containerization: Use containers (Docker, Kubernetes) for consistent deployment across environments with more efficient resource utilization than traditional virtualization.
Managed services: Leverage cloud provider managed databases, analytics platforms, and AI/ML services rather than operating infrastructure. Providers optimize these services for efficiency at scale.
Auto-scaling policies: Implement intelligent auto-scaling that responds to actual demand:
- Scale down development/test environments during non-business hours
- Reduce analytical environment capacity during clinical peak hours
- Scale up patient portal and scheduling systems during business hours, scale down overnight
Storage lifecycle policies: Implement automated data lifecycle management:
- Move infrequently accessed data to lower-cost, lower-energy storage tiers
- Delete temporary data on defined schedules
- Compress and deduplicate where appropriate
Practice example: Providence St. Joseph Health redesigned its patient engagement platform using microservices and serverless architecture on AWS, reducing compute resource consumption by 70% while improving responsiveness and scalability.
Select Regions Based on Sustainability Criteria
Not all cloud regions offer equivalent sustainability characteristics:
Evaluate renewable energy percentage: Cloud providers publish renewable energy data by region. Google Cloud’s region picker shows carbon-free energy percentage, with regions like Iowa at 96% while Singapore is only 6%.
Consider Power Usage Effectiveness (PUE): Newer cloud regions typically achieve better PUE than older facilities. Google’s Hamina, Finland data center achieves PUE of 1.08 through seawater cooling.
Balance latency and sustainability: For workloads without strict latency requirements (analytics, training environments, long-term archival), select most sustainable regions even if geographically distant.
Multi-region strategies: For applications requiring geographic redundancy, select regions with high renewable energy percentages rather than simply choosing closest regions.
Data residency compliance: Some healthcare data has legal residency requirements. Work within those constraints but optimize sustainability within permissible regions.
Practice example: UC Davis Health selected Google Cloud’s Iowa region for research computing workloads despite being based in California, prioritizing the region’s 96% carbon-free energy over minimal latency benefits from closer regions.
Implement FinOps Practices for Cost and Sustainability
Cloud financial management (FinOps) and sustainability optimization are closely aligned:
Resource tagging: Implement comprehensive tagging to identify resource ownership, application, environment, and cost center. This enables detailed analysis of cost and carbon footprint by department or application.
Right-sizing discipline: Regularly review resource utilization and adjust sizing:
- Use AWS Compute Optimizer, Azure Advisor, or Google Cloud Recommender
- Establish quarterly right-sizing reviews
- Set policies requiring resource utilization justification above defined thresholds
Reserved capacity for steady-state workloads: Use reserved instances or savings plans for predictable workloads to reduce costs by 40-60% while improving provider resource planning for sustainability.
Spot instances for fault-tolerant workloads: Use spot/preemptible instances for research computing, batch processing, and other interruptible workloads to reduce costs by 60-90% while consuming provider excess capacity.
Automated resource cleanup: Implement policies that automatically delete or stop resources:
- Development environments stopped after 8 hours of inactivity
- Test data deleted after 30 days
- Unused storage volumes deleted after 7 days detached
Practice example: Intermountain Healthcare implemented comprehensive FinOps practices reducing cloud costs by 34% in the first year while simultaneously reducing carbon footprint by 42% through improved resource efficiency.
Establish Cloud Center of Excellence
Successful healthcare cloud adoption requires centralized expertise and governance:
Cross-functional team composition:
- Cloud architects with healthcare experience
- Security and compliance specialists
- Application developers
- FinOps/cost management experts
- Clinical informatics representatives
Responsibilities include:
- Develop cloud architecture standards and reference patterns
- Create security and compliance guardrails
- Provide consulting and architecture review for projects
- Manage cost optimization and sustainability metrics
- Establish training programs and knowledge sharing
- Vendor management and cloud provider relationship
Governance framework:
- Project approval process including sustainability impact assessment
- Architecture review checkpoints at key project phases
- Post-implementation review to capture lessons learned
- Exception process for unique requirements
Practice example: Mass General Brigham’s cloud center of excellence reviews all cloud projects during planning phase, providing architecture guidance and ensuring alignment with sustainability and cost objectives. Projects must demonstrate expected carbon footprint impact for approval.
Partner with Cloud-Experienced Healthcare Consultants
Healthcare cloud migration complexity often requires external expertise:
Consultant selection criteria:
- Healthcare-specific cloud experience (not just general cloud expertise)
- HIPAA compliance and healthcare security expertise
- Demonstrated sustainability focus in methodology
- References from comparable healthcare organizations
Engagement models:
- Strategy and planning: Help develop cloud strategy aligned with organizational goals
- Migration execution: Hands-on support for complex application migrations
- Managed services: Ongoing cloud operations and optimization
- Staff augmentation: Temporary expertise while building internal capabilities
Knowledge transfer focus: Ensure consultant engagements include formal knowledge transfer to build internal capabilities rather than creating permanent dependencies.
Practice example: Advocate Aurora Health partnered with a healthcare-specialized cloud consultant for initial Azure migration strategy and first wave of application migrations, with explicit knowledge transfer requirements. Internal team assumed full responsibility by second wave with consultant available for advisory support.
Future Trends in Green Cloud Healthcare
Carbon-Aware Computing and Regional Optimization
Emerging technologies will enable more sophisticated approaches to minimizing cloud carbon footprint:
Carbon-aware workload scheduling: Cloud platforms are developing capabilities to schedule flexible workloads (analytics, batch processing, machine learning training) during times when renewable energy availability is highest on the grid.
Google Cloud has introduced carbon-aware load shifting that moves delay-tolerant workloads to times and regions where carbon-free energy percentage is highest. Early implementations show 10-15% additional carbon reduction beyond static region selection.
Healthcare applications: Large-scale genomic analysis, claims processing, population health analytics, and machine learning model training could shift to high-renewable-energy periods without impacting clinical operations.
Expected timeline: Basic carbon-aware scheduling available now with increasing sophistication over next 2-3 years. Healthcare adoption likely 3-5 years as platforms mature and healthcare IT develops expertise.
Liquid Cooling and Advanced Thermal Management
Next-generation data center cooling technologies will dramatically improve energy efficiency:
Direct-to-chip liquid cooling: Circulating liquid directly to processor heat exchangers rather than cooling entire rooms. This approach reduces cooling energy by 40-50% versus advanced air cooling.
Immersion cooling: Submerging servers in non-conductive liquid provides even more efficient heat removal, particularly for high-density AI/ML infrastructure.
Healthcare impact: As cloud providers deploy these technologies in new data centers, healthcare workloads automatically benefit. Providers with immersion-cooled AI infrastructure offer more sustainable options for medical imaging analysis, natural language processing, and predictive analytics.
Expected timeline: Cloud providers are deploying liquid cooling in new facilities now. Widespread deployment across major regions within 3-5 years.
Edge Computing for Healthcare IoT
Edge computing architectures process data closer to generation sources, reducing data transmission and central processing:
Healthcare edge applications:
- Real-time patient monitoring with local processing, transmitting only clinically significant events
- Medical imaging preliminary processing at modality or department level
- Smart hospital systems (HVAC, lighting, access control) with local automation
- Remote clinics with local computing for basic operations and cloud connectivity for complex cases
Sustainability benefits:
- Reduced network energy consumption from decreased data transmission
- Improved local efficiency through real-time optimization
- Continued operation during network disruptions without energy-intensive failover systems
Expected timeline: Healthcare edge computing deployments accelerating now. Mainstream adoption for appropriate use cases within 2-4 years.
AI-Optimized Infrastructure
Purpose-built AI infrastructure will reduce energy consumption for healthcare’s growing AI/ML workloads:
Specialized processors: TPUs (Tensor Processing Units), AI accelerators, and neuromorphic computing chips deliver 5-10x better performance per watt than general-purpose processors for AI workloads.
Model efficiency: Techniques like quantization, pruning, and knowledge distillation reduce model size and computational requirements by 80-90% with minimal accuracy impact.
Healthcare applications: Radiology AI, pathology analysis, clinical decision support, sepsis prediction, and population health analytics all benefit from more efficient AI infrastructure.
Sustainability impact: Training a large language model can consume 500+ megawatt-hours of electricity. More efficient infrastructure and techniques reduce this by 90%+.
Expected timeline: AI-specialized infrastructure available now with rapid capability expansion. Healthcare adoption accelerating as regulatory frameworks for AI in healthcare mature.
Sustainable Hardware and Circular Economy
Cloud providers are pioneering circular economy approaches to hardware:
Extended hardware lifecycles: Rather than 3-5 year replacement cycles, cloud providers operate servers 6-8+ years through strategic workload placement and component upgrades.
Component reuse: Harvesting functional components from decommissioned servers for remanufacturing or spare parts.
Sustainable materials: Increasing use of recycled materials in manufacturing and reduction of rare earth elements.
Zero waste goals: Microsoft committed to zero waste certification for data centers by 2030. Google aims for net-zero waste by 2030.
Healthcare benefit: By using cloud services, healthcare organizations automatically benefit from these circular economy practices without managing complex programs internally.
Green Software Engineering Practices
Software development practices will increasingly emphasize efficiency and sustainability:
Carbon-aware development: Tools and frameworks that provide developers real-time feedback on code energy consumption.
Efficient algorithms: Optimization for computational efficiency (reducing CPU cycles) directly correlates with energy efficiency.
Sustainability in procurement: Healthcare organizations will include sustainability criteria in software procurement alongside functionality and cost.
Healthcare-specific tools: Development frameworks optimized for common healthcare workflows (HL7 processing, FHIR implementations, clinical decision support).
Expected timeline: Green software engineering emerging now in leading organizations. Mainstream healthcare adoption likely 5-7 years.
Conclusion: Strategic Imperative for Healthcare IT Leaders
Green Cloud in Healthcare represents far more than an environmental initiative—it’s a strategic transformation that simultaneously addresses sustainability goals, cost pressures, operational resilience, and innovation capacity. Healthcare IT leaders face an increasingly clear choice: maintain energy-intensive, inefficient on-premises infrastructure or leverage hyperscale cloud platforms that deliver superior sustainability, security, and capabilities.
The evidence is compelling: healthcare organizations successfully implementing green cloud strategies achieve 65-85% reduction in IT-related carbon emissions while realizing 30-40% cost savings, improving disaster recovery capabilities, and accelerating innovation. These aren’t theoretical benefits—organizations like Mass General Brigham, UC San Diego Health, and Providence St. Joseph Health have demonstrated measurable results at scale.
Key takeaways for healthcare IT leaders:
1. Sustainability and business performance align: Green cloud isn’t a trade-off between environmental responsibility and financial performance. The same characteristics that reduce carbon emissions—efficient resource utilization, renewable energy, extended hardware lifecycles—also reduce costs and improve operational efficiency.
2. Start with measurement: Baseline your current IT carbon footprint, establish measurable goals, and track progress quarterly. Use cloud provider tools to maintain visibility into ongoing emissions.
3. Adopt phased approach: Begin with cloud-ready applications (collaboration, analytics, administrative systems) to build expertise before migrating complex clinical systems. Quick wins build organizational confidence and demonstrate value.
4. Prioritize cloud-native architecture: Maximize sustainability benefits through microservices, serverless computing, intelligent auto-scaling, and storage lifecycle management. Simply “lifting and shifting” on-premises architectures to cloud leaves substantial benefits unrealized.
5. Select regions strategically: Renewable energy percentages vary dramatically across cloud regions. For workloads without strict latency requirements, prioritize sustainability in region selection.
6. Build internal capabilities: Invest in cloud training, establish a cloud center of excellence, and develop FinOps practices. External consultants provide valuable support but long-term success requires internal expertise.
7. Consider hybrid reality: Few healthcare organizations achieve 100% cloud migration in the near term. Design thoughtful hybrid architectures that optimize workload placement while providing pathway to increased cloud adoption.
8. Engage clinical leadership: Cloud migration affects clinical workflows and requires clinical stakeholder engagement. Communicate benefits (improved disaster recovery, faster innovation, enhanced security) alongside technical implementation.
As healthcare grapples with climate change’s direct health impacts—from respiratory disease to heat-related illness to the spread of infectious diseases—IT infrastructure’s environmental footprint becomes an ethical issue, not just an operational one. Organizations that lead in green cloud adoption position themselves as sustainability leaders while achieving superior business results.
The question for healthcare IT leaders isn’t whether to pursue green cloud strategies, but how quickly you can responsibly execute migration to maximize sustainability impact, cost reduction, and operational benefits. The technology is proven, the business case is clear, and the environmental imperative is urgent.
Healthcare exists to improve human health. Reducing the industry’s carbon footprint through green cloud adoption directly serves that mission while strengthening organizational resilience and financial performance. The time to act is now.
About RizeX Labs
At RizeX Labs, we help healthcare organizations modernize their IT infrastructure using scalable, secure, and sustainable cloud solutions.
Our expertise spans cloud architecture, Salesforce implementations, and healthcare system integrations—enabling hospitals to transition from outdated, energy-intensive systems to efficient, cloud-based environments.
We focus on building solutions that not only improve operational efficiency but also support sustainability goals by reducing carbon emissions and optimizing resource utilization.
Internal Links:
- Salesforce Admin & Development Training
- Remote Patient Monitoring (RPM) in Salesforce Health Cloud: Transforming Connected Healthcare Delivery
- How to Use AI in Salesforce Health Cloud for Predictive Patient Care (Einstein + Real Use Cases)
- New Releases in Salesforce Health Cloud Spring ’26: What Healthcare Organizations Need to Know
- How to Customize Salesforce Health Cloud Using Lightning Web Components (LWC) for Healthcare Use Cases
- 30 Essential Questions About Salesforce Health Cloud Answered: Beginner to Advanced Guide
- Salesforce Sales Cloud vs Health Cloud: The Strategic CRM Decision That Defines Your Healthcare Business Trajectory
- Using Salesforce Health Cloud for Insurance & Claims Coordination: Beyond the Hospital Walls
External Links:
- Salesforce Official Website
- Salesforce Health Cloud Overview
- Salesforce Revenue Cloud Overview
- Salesforce AppExchange (CLM tools)
- Salesforce CPQ Documentation
Quick Summary
Green Cloud in Healthcare offers a transformative solution to reduce hospital carbon footprints while improving IT performance and reducing costs. By migrating from energy-intensive on-premises data centers to hyperscale cloud infrastructure powered by renewable energy, healthcare organizations achieve 65-85% reduction in IT-related carbon emissions and 30-40% cost savings over 3-5 years. Major cloud providers (AWS, Azure, Google Cloud) operate with Power Usage Effectiveness (PUE) ratings of 1.1-1.2 compared to traditional hospital data centers at 1.8-2.0, while matching 80-100% of energy consumption with renewable sources. Beyond sustainability, green cloud delivers critical business benefits including enhanced disaster recovery, improved scalability for AI and analytics workloads, and HIPAA-compliant security that exceeds most on-premises capabilities. Leading healthcare systems like Mass General Brigham, UC San Diego Health, and Providence St. Joseph Health have demonstrated measurable results, eliminating thousands of metric tons of CO2 emissions annually while accelerating innovation and strengthening operational resilience. While challenges exist—including application compatibility, data migration complexity, and skills gaps—phased implementation approaches starting with non-production environments and cloud-ready applications enable healthcare organizations to build expertise while delivering quick wins. For healthcare IT leaders balancing sustainability commitments, cost pressures, and the need for advanced capabilities to support value-based care and population health, green cloud represents not just an environmental initiative but a strategic imperative that aligns organizational mission with operational excellence.


