Introduction :
The Salesforce Health Cloud y stands at a critical intersection where technology, regulatory compliance, and patient expectations converge. While much of the conversation around digital transformation in healthcare focuses on clinical outcomes and patient engagement, there’s a massive operational challenge that remains largely underserved: the complex choreography between payers, providers, and third-party administrators in managing insurance verification, authorization, and claims coordination.
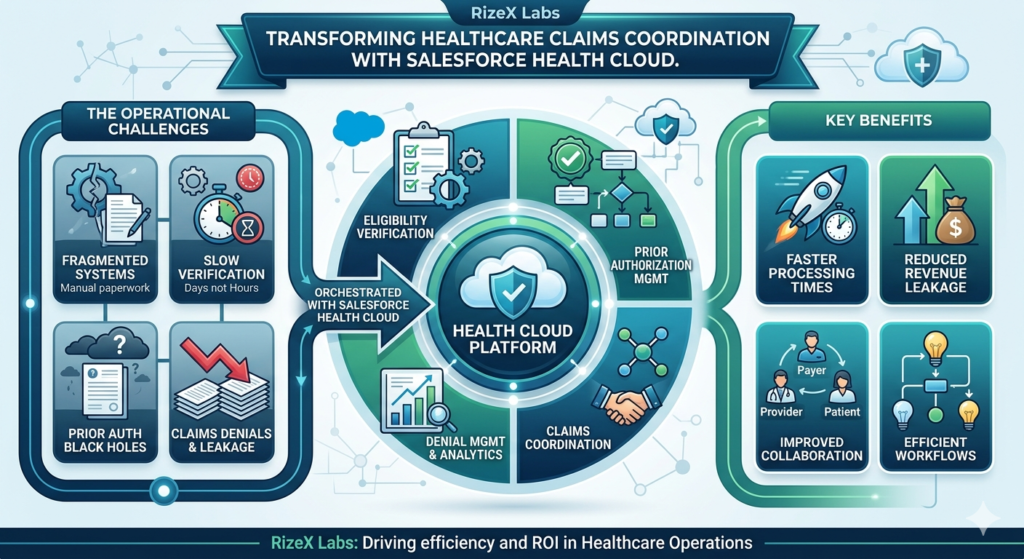
At RizeX Labs, we’ve observed a persistent pattern across healthcare organizations—brilliant clinical systems that somehow lose efficiency the moment a claim enters the picture. Insurance verification takes days instead of hours. Prior authorizations become black holes of communication. Claims denials trigger manual research that pulls staff away from patient-facing activities. The result? Revenue leakage, administrative burnout, and deteriorating relationships between healthcare organizations and their payer partners.
Salesforce Health Cloud has evolved significantly beyond its origins as a patient relationship management platform. Today, it represents a powerful ecosystem for orchestrating the entire insurance and claims lifecycle—from eligibility verification through final remittance processing. This blog explores how forward-thinking healthcare organizations and insurers are leveraging Health Cloud to transform their most inefficient administrative processes into competitive advantages.
We’ll examine the specific insurance and claims coordination challenges that keep CFOs and operations leaders awake at night, detail how Health Cloud’s architecture addresses these problems, and present real-world implementations that have delivered measurable ROI. Whether you’re a health system struggling with claim denials, an insurance company seeking better provider collaboration, or a Salesforce decision-maker evaluating Health Cloud’s fit for your organization, this deep dive will provide the strategic and tactical insights you need.
The Problem Statement: Where Insurance Workflows Break Down
The Fragmentation Challenge
Healthcare organizations typically operate claims and insurance coordination across multiple disconnected systems: separate platforms for eligibility verification, authorization management, claims submission, denial tracking, and payment posting. Each system maintains its own data structure, requiring manual reconciliation and creating numerous opportunities for errors.
Consider a typical scenario: A specialty clinic verifies insurance eligibility in one system, documents the authorization in another, submits the claim through a clearinghouse, tracks denials in spreadsheets, and manages appeals through email threads. When a payer calls about a claim, staff members must access three or four different systems to piece together the complete story. This fragmentation doesn’t just waste time—it creates invisible revenue leaks where claims fall through the cracks entirely.
The Information Asymmetry Problem
Payers and providers operate with fundamentally different information sets and priorities. Providers focus on clinical documentation and service delivery, often treating claims as an afterthought. Payers concentrate on medical necessity, contractual compliance, and fraud prevention. This information asymmetry creates friction at every touchpoint.
When prior authorization requests lack the specific clinical details payers require, they get denied or delayed. When providers don’t understand the specific denial reasons (buried in cryptic claim adjustment reason codes), they can’t effectively appeal. When neither party has visibility into where a claim sits in the review process, both resort to phone calls and portal logins that drain productivity on both sides.
The Claims Denial Crisis
Industry data consistently shows that 5-10% of all claims are initially denied, with some specialties and payers experiencing rates above 15%. More concerning is that only 60-70% of denials ever get appealed, and of those appeals, many are filed beyond timely filing limits. The financial impact is staggering—a mid-sized hospital can lose millions annually to preventable denials and unworked rejections.
The root cause isn’t a lack of effort. Dedicated revenue cycle teams work exhaustively to prevent and overturn denials. The problem is that denial prevention and resolution happens reactively, after the damage is done. Without predictive intelligence about which claims carry denial risk before submission, and without streamlined workflows to work denials efficiently, healthcare organizations fight an uphill battle.
The Prior Authorization Bottleneck
Prior authorization represents one of the most frustrating administrative burdens in healthcare. A 2022 American Medical Association survey found that physicians and their staff complete an average of 41 prior authorizations per physician per week, requiring nearly two business days of physician and staff time.
The process typically involves: identifying which services require authorization, gathering clinical documentation, submitting requests through payer-specific portals or fax, tracking request status, following up on pending requests, and documenting authorization details for billing. Each step introduces delays and potential breakdowns. Urgent procedures get postponed. Patients become frustrated. Providers write off services that technically required authorization but were delivered emergently.
The Coordination Gap in Value-Based Arrangements
As healthcare shifts toward value-based reimbursement, insurance coordination becomes exponentially more complex. Providers must now track not just individual claim payments but aggregate quality metrics, risk-adjusted patient panels, shared savings calculations, and complex bundled payment methodologies.
Traditional claims management systems were built for fee-for-service volume tracking. They lack the analytical capabilities to monitor value-based contract performance, identify care gaps that affect quality scores, or coordinate across the multiple providers involved in bundled episodes. This leaves healthcare organizations flying blind in arrangements where financial performance depends on sophisticated coordination.
The Member Experience Disconnect
From the patient’s (or member’s) perspective, insurance coordination represents a confusing maze. They don’t understand why their provider can’t simply tell them whether a service is covered. They receive separate bills from the provider and insurer without context. When problems arise, they’re shuttled between the provider’s billing department and the payer’s customer service with each pointing to the other.
This poor experience doesn’t just create patient dissatisfaction—it generates operational costs. Both providers and payers field countless phone calls from confused members asking about claim status, coverage details, and billing questions that could be prevented through better coordination and transparency.
The Solution: Salesforce Health Cloud as a Unified Insurance Coordination Platform
Salesforce Health Cloud provides a fundamentally different architectural approach to insurance and claims coordination. Rather than treating these processes as back-office functions separate from member and provider relationships, Health Cloud creates a unified platform where insurance workflows, clinical context, and relationship management converge.
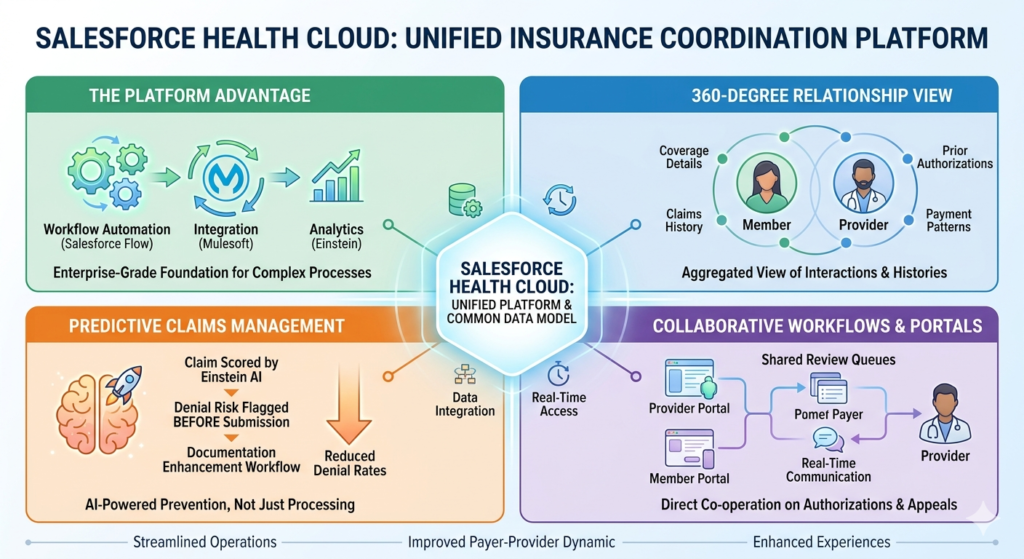
The Platform Architecture Advantage
Health Cloud sits on the Salesforce Platform, which means it inherits enterprise-grade capabilities for workflow automation, integration, analytics, and user experience that would take years to build in a purpose-built claims system. Organizations can leverage Salesforce Flow for complex business process automation, Einstein Analytics for predictive insights, and Mulesoft for integration—all within a unified data model.
This architectural foundation matters enormously for insurance coordination. When eligibility verification, authorization tracking, claims submission, denial management, and payment posting all occur within the same platform sharing a common data model, the fragmentation problem dissolves. Every stakeholder—from the patient access representative verifying coverage to the revenue cycle analyst working denials—operates from the same source of truth.
The 360-Degree View of Insurance Relationships
Health Cloud’s core value proposition is creating a comprehensive view of healthcare relationships. For insurance coordination, this means aggregating insurance data, claims history, authorization records, payment patterns, and communication history into a single member or provider profile.
When a care coordinator opens a member record, they instantly see active insurance policies, pending authorizations, recent claims, outstanding balances, and previous coordination challenges. When a provider relations specialist reviews a network provider, they see claim submission patterns, denial rates by claim type, average payment timelines, and documentation quality trends. This context transforms every interaction from a transactional exchange to an informed conversation.
From Reactive to Predictive Claims Management
Health Cloud’s integration with Einstein AI enables organizations to shift from reactive claims processing to predictive denial prevention. By analyzing historical claim data, denial patterns, payer-specific requirements, and clinical documentation, Einstein can score claims for denial risk before submission.
A high-risk score for missing documentation triggers an automated workflow routing the claim to a specialist for review and documentation enhancement before submission. Patterns of denials for specific procedure-diagnosis combinations automatically generate alerts for front-end staff during scheduling. This predictive approach doesn’t just reduce denials—it reduces the costly rework of appeals and resubmissions.
Collaborative Workflows That Cross Organizational Boundaries
One of Health Cloud’s most powerful yet underutilized capabilities is its support for collaborative workflows that span organizational boundaries. Using Salesforce Experience Cloud, payers and providers can create secure portals where they collaborate on prior authorizations, claims resolution, and care coordination within shared workflows.
Instead of a provider submitting an authorization request into a black box, they submit it into a shared workspace where they can see exactly where it sits in the payer’s review queue, what additional information is needed, and communicate directly with the reviewing clinician. Instead of submitting a claim appeal through fax or portal upload, they work the appeal in a collaborative workspace where both parties can see the complete claim history and exchange information in real-time.
This collaborative approach fundamentally changes the payer-provider dynamic from adversarial to cooperative, reducing resolution times and improving outcomes for both parties.
Unified Member and Provider Portals
Health Cloud enables organizations to create sophisticated self-service portals for both members and network providers. Members can check their coverage details, view claim status, understand their financial responsibility, and resolve billing questions without calling customer service. Providers can verify eligibility, check authorization status, submit claims, view remittance details, and communicate with payer representatives.
These portals aren’t separate systems bolted onto Health Cloud—they’re native extensions of the platform, with full access to the underlying data model and workflow engine. When a member updates their address in the portal, that change immediately flows to all insurance coordination processes. When a provider submits additional documentation through the portal, it’s instantly available to the claims examiner reviewing the case.
Key Features for Insurance and Claims Coordination
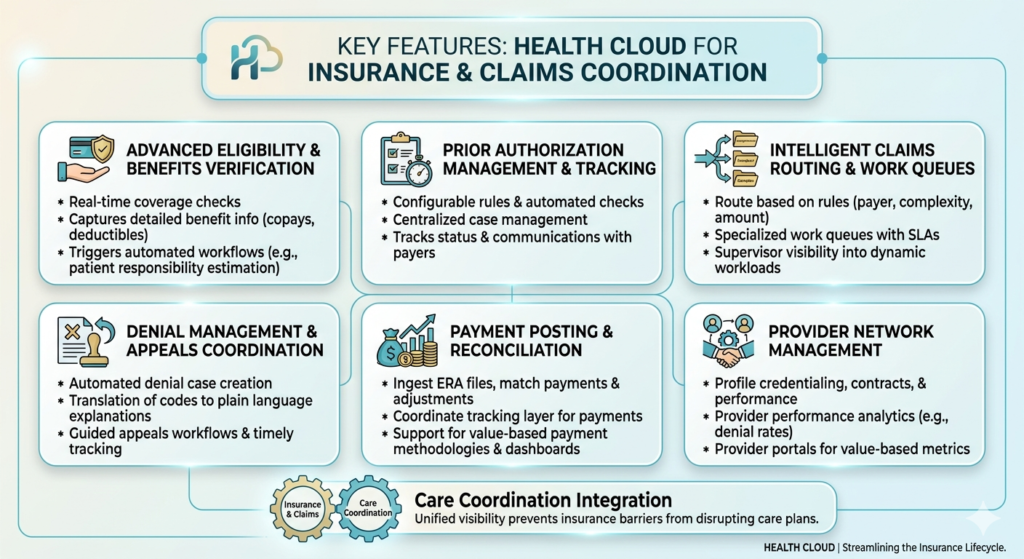
Advanced Eligibility and Benefits Verification
Health Cloud can integrate with real-time eligibility verification services, automatically checking coverage details during scheduling or registration and storing the results in the member’s profile. Beyond simple active/inactive coverage checks, the system can capture detailed benefit information: copays, deductibles, out-of-pocket maximums, coverage limitations, and service-specific requirements.
More importantly, Health Cloud can trigger automated workflows based on eligibility results. If a member’s deductible hasn’t been met, the system can calculate estimated patient responsibility and trigger communication workflows to discuss payment options before the service. If coverage requires prior authorization, the system automatically initiates the authorization workflow and prevents appointment confirmation until authorization is secured.
Healthcare organizations using this capability report dramatic reductions in bad debt and insurance-related patient dissatisfaction, as surprises at time of service or billing become the exception rather than the norm.
Prior Authorization Management and Tracking
Health Cloud provides a comprehensive framework for managing the complete prior authorization lifecycle. Authorization requirements can be configured by payer, service type, and patient characteristics, with automated checking during scheduling or order entry. When authorization is required, the system creates an authorization case that routes to the appropriate team with all necessary clinical documentation attached.
Staff can track authorization status, set follow-up reminders, and document communications with the payer—all within the authorization record. Integration with payer portals (where available) enables automated status checking. When authorization is approved, denied, or modified, the system updates the member’s profile and notifies relevant staff.
For organizations managing high volumes of authorizations, this centralization and automation can reduce processing time per authorization by 50% or more while dramatically reducing the risk of delivering services without proper authorization.
Intelligent Claims Routing and Work Queues
Not all claims require the same level of expertise to process. Straightforward claims for established payers and service types should move through quickly with minimal touches. Complex claims involving multiple payers, unusual procedures, or high-dollar amounts require experienced specialists.
Health Cloud enables sophisticated claims routing based on configurable business rules. Claims can be automatically routed to specialized work queues based on payer, service type, claim amount, complexity score, or denial risk score. Each queue can have defined service level agreements, with escalation workflows triggering if claims age beyond thresholds.
Supervisors gain real-time visibility into queue volumes, aging, and staff productivity, enabling dynamic workload balancing and identifying bottlenecks before they impact cash flow.
Denial Management and Appeals Coordination
When claims are denied, Health Cloud can automatically create denial cases with all relevant claim details, denial reasons, and supporting documentation attached. Denial reason codes are translated into plain language explanations, and the system can suggest appropriate corrective actions based on the denial reason and historical resolution patterns.
Appeals workflows guide staff through the appeal process, ensuring all payer-specific requirements are met and timely filing deadlines are tracked. For denials that require additional clinical documentation, the system can route requests to the appropriate clinician with specific details about what information is needed and why.
Analytics dashboards track denial rates by payer, service type, denial reason, and staff member, enabling targeted process improvements. When patterns emerge—such as a specific payer consistently denying a particular procedure-diagnosis combination—the system can alert leadership to pursue contract clarification or modify front-end processes.
Payment Posting and Reconciliation
While Health Cloud isn’t a replacement for practice management or revenue cycle management systems, it can serve as a coordination layer for payment tracking and reconciliation. Electronic remittance advice (ERA) files can be ingested, parsed, and matched to claim records, with payment details and contractual adjustments stored in the member and claim history.
For value-based arrangements with complex payment methodologies, Health Cloud’s flexible data model can track incentive payments, withhold distributions, shared savings calculations, and quality metric performance. Organizations can create dashboards that show real-time performance against value-based contract targets, enabling proactive intervention before performance periods close.
Provider Network Management
For payers and accountable care organizations managing provider networks, Health Cloud offers robust provider relationship management capabilities. Provider profiles can store credentialing information, contract terms, performance metrics, and communication history.
Claims data flowing through Health Cloud enables sophisticated provider performance analytics: claim submission quality, documentation completeness, average charge-to-reimbursement ratios, denial rates, and compliance with coding guidelines. These insights inform provider education initiatives, contract negotiations, and network adequacy assessments.
For value-based arrangements, provider portals can show individual providers their performance against quality metrics and cost targets, with drill-down capabilities to identify specific patients or service categories driving results.
Care Coordination Integration
While this blog focuses on the insurance and claims aspects of Health Cloud, it’s worth noting that these capabilities integrate seamlessly with Health Cloud’s care coordination features. When a care manager is coordinating services for a complex patient, they have immediate visibility into insurance coverage, authorization status, and claims history.
This integration prevents a common breakdown point: care coordination creating plans that are never executed because insurance barriers weren’t identified until time of service. With unified visibility, care coordinators can proactively address insurance obstacles as part of care planning.
Real-World Use Case: Multi-Specialty Group Transforms Revenue Cycle Operations
The Organization
A large multi-specialty physician group operating 40 locations across three states with approximately 300 physicians and 650,000 annual patient encounters. The organization participated in multiple value-based contracts with commercial and Medicare Advantage payers while maintaining significant fee-for-service volume.
The Challenges
Prior to implementing Health Cloud, the organization faced mounting revenue cycle pressures:
- Prior authorization delays: Processing authorizations required 3-5 business days on average, causing appointment delays and patient frustration. The organization employed 12 full-time staff members dedicated to authorization processing, yet the backlog continued growing.
- Claims denial rate: Overall denial rate exceeded 12%, significantly above industry benchmarks. Denials for lack of prior authorization, medical necessity, and timely filing were most common. Less than 55% of denials were successfully appealed.
- Fragmented systems: Staff worked across six different systems to manage the revenue cycle: the EHR for clinical documentation, a practice management system for claims submission, separate portals for each major payer, spreadsheets for authorization tracking, and email for internal coordination and external communication.
- Limited value-based contract visibility: The organization participated in four value-based contracts representing approximately $45 million in annual revenue, but lacked integrated tools to track performance. Finance staff spent days each month manually compiling data from various sources to assess contract performance.
- Provider frustration: Physicians received frequent inquiries from billing staff about documentation for denied claims, pulling them away from patient care. Many expressed frustration that administrative burdens were increasing despite promised efficiencies from new technology.
The Health Cloud Implementation
Working with RizeX Labs, the organization implemented a comprehensive Health Cloud solution focused on insurance and claims coordination:
Phase 1: Foundation and Eligibility (Months 1-3)
- Integrated Health Cloud with the existing EHR and practice management system using Mulesoft
- Implemented real-time eligibility verification integrated with scheduling workflows
- Created unified member profiles consolidating insurance information, authorization history, and claims data
- Developed provider portal for eligibility checking and authorization status inquiry
Phase 2: Prior Authorization Management (Months 4-6)
- Configured authorization requirements by payer and service type
- Built automated workflows for authorization request submission, tracking, and follow-up
- Created specialized work queues for complex authorizations requiring clinical review
- Implemented payer portal integrations for automated status checking
Phase 3: Claims Intelligence and Denial Management (Months 7-9)
- Implemented Einstein AI for pre-submission denial risk scoring
- Created automated denial case generation and routing workflows
- Built appeals management capabilities with timely filing tracking
- Developed comprehensive denial analytics dashboards
Phase 4: Value-Based Contract Management (Months 10-12)
- Designed custom objects to track value-based contract terms and performance
- Implemented automated quality metric tracking and care gap identification
- Created provider-facing dashboards showing individual performance against contract targets
- Built workflows to coordinate interventions for at-risk contract performance
The Implementation Approach
Several factors contributed to the implementation’s success:
Executive sponsorship: The CFO and CMO served as co-sponsors, ensuring both financial and clinical perspectives informed solution design.
Phased rollout: Rather than a big-bang approach, the organization rolled out capabilities in phases, allowing staff to adapt and providing opportunities to refine workflows based on real-world usage.
Revenue cycle staff involvement: Front-line staff who would use the system daily participated in design sessions, workflow testing, and training development. This ensured the solution addressed actual pain points and gained user adoption.
Integration strategy: Rather than attempting to replace all existing systems, Health Cloud served as an orchestration layer, integrating with the EHR and practice management system while providing unified visibility and workflow management.
Change management investment: The organization allocated significant resources to training, communication, and ongoing support during the transition period, recognizing that technology alone wouldn’t drive results without process change.
The Results
After twelve months of full operation, the organization documented substantial improvements:
Operational Efficiency
- Prior authorization processing time decreased from 3-5 business days to 1.2 business days on average
- Authorization staff reduced from 12 FTEs to 7 FTEs through automation and efficiency gains
- Staff reported spending 40% less time accessing multiple systems and manually reconciling information
- Physicians reported 60% reduction in interruptions for claims-related documentation requests
Financial Performance
- Claims denial rate decreased from 12.1% to 6.8%
- Appeal success rate increased from 55% to 78%
- Clean claim rate (claims paid on first submission) improved from 81% to 92%
- Days in accounts receivable decreased from 48 to 38 days
- Net revenue improvement of $4.2 million annually, directly attributable to denial reduction and improved authorization compliance
Value-Based Contract Performance
- Quality metric performance improved across all four value-based contracts, driven by better care gap identification and coordination
- The organization achieved maximum shared savings under three of four contracts, resulting in $1.8 million in additional revenue
- Contract performance reporting time reduced from 3 days per month to real-time access through dashboards
Member and Provider Experience
- Patient complaints related to insurance and billing decreased by 45%
- Network provider satisfaction scores (measured through periodic surveys) improved by 23 points
- Self-service portal adoption reached 34% of active patients, deflecting an estimated 850 customer service calls monthly
ROI Analysis
- Total implementation cost (software, implementation services, internal resources): $1.2 million
- Annual operational cost (licenses, support, maintenance): $320,000
- Year-one quantified benefits: $6.0 million (revenue improvement, cost reduction, and efficiency gains)
- Simple payback period: 2.4 months
- Three-year ROI: 1,275%
Key Success Factors
The organization’s leadership identified several factors that drove successful outcomes:
Data quality focus: Significant effort went into cleaning and standardizing insurance data before implementation, ensuring Health Cloud had reliable information to work with.
Workflow redesign: Rather than simply automating existing processes, the organization used the implementation as an opportunity to redesign workflows around best practices.
Continuous improvement mindset: The organization established a monthly review cadence to examine analytics, identify opportunities for further optimization, and refine system configuration.
Stakeholder communication: Regular updates to physicians, staff, and leadership kept everyone informed about progress and created opportunities to address concerns early.
Business Impact and ROI Considerations
Healthcare organizations and insurers evaluating Health Cloud for insurance coordination should consider multiple dimensions of business impact beyond simple cost reduction.
Revenue Acceleration
Improved authorization management and reduced denials directly accelerate cash flow. When claims are submitted cleanly the first time with appropriate authorizations and supporting documentation, they’re adjudicated faster and paid sooner. This improvement in days in accounts receivable can free up significant working capital, reducing the need for credit lines or enabling redeployment of capital to strategic investments.
For organizations operating on tight margins, this acceleration can be transformative. A 10-day reduction in days in accounts receivable for a $500 million revenue organization frees up nearly $14 million in working capital.
Margin Protection
Denied claims that never get appealed, services delivered without authorization, and timely filing limit expirations represent pure margin leakage. Health Cloud’s systematic approach to denial prevention and management plugs these leaks.
Beyond direct denial reduction, the platform enables more strategic contract management. With visibility into payment patterns, contractual allowables versus actual reimbursements, and service-line profitability by payer, organizations can make better decisions about contract negotiations and network participation.
Operational Efficiency
Revenue cycle operations are labor-intensive, and labor costs continue rising. Automation of routine tasks—eligibility verification, authorization status checking, claim submission, and payment posting—enables organizations to manage growing volume without proportional increases in staffing.
More importantly, automation allows staff to focus on high-value activities. Instead of manually checking authorization status, staff can focus on resolving complex denials, improving provider documentation, and optimizing payer relationships. This shift from transaction processing to strategic value creation represents the real efficiency opportunity.
Strategic Capabilities for Value-Based Care
As reimbursement continues shifting toward value-based arrangements, organizations need capabilities that traditional claims systems never contemplated. Tracking quality metrics, coordinating care across multiple providers, identifying and closing care gaps, and managing financial risk all require sophisticated data integration and analytics.
Health Cloud’s platform architecture and native analytics capabilities position organizations to succeed in value-based arrangements. Rather than purchasing separate population health management systems, care coordination platforms, and contract management tools, organizations can build these capabilities on a unified foundation.
The strategic value of this unified approach increases over time. As value-based arrangements grow more sophisticated—incorporating social determinants of health, requiring integration with community resources, and demanding longitudinal patient engagement—the organization’s investment in Health Cloud as a foundation continues paying dividends.
Competitive Differentiation
In increasingly competitive healthcare markets, operational excellence in revenue cycle and insurance coordination creates competitive advantages. Health systems that can provide real-time insurance verification, transparent cost estimates, and smooth authorization processes deliver better patient experiences than competitors struggling with these basics.
For payers, superior provider collaboration through shared workflows and transparent communication differentiates their products in the market. When providers find it easier to work with a particular payer—faster authorization decisions, clearer denial explanations, collaborative problem-solving—they’re more likely to participate in narrow network products and steer patients toward that payer’s plans.
Risk Mitigation
Healthcare operates in a heavily regulated environment where compliance failures carry severe consequences. Health Cloud’s comprehensive audit trail, workflow automation, and documentation capabilities reduce compliance risk across multiple dimensions.
Prior authorization tracking ensures services aren’t delivered without appropriate approvals. Appeals management ensures timely filing deadlines are met. Documentation requirements are systematically tracked and enforced. When regulators or payers audit the organization, complete documentation is readily available rather than scattered across systems and file cabinets.
Quantifying ROI
Organizations building the business case for Health Cloud should consider these quantifiable benefit categories:
Direct Revenue Impact
- Denial reduction (reduction in denial rate × annual claim volume × average claim amount)
- Improved appeal success (increase in appeal success rate × denied claim volume × average claim amount)
- Authorization compliance (reduction in services delivered without authorization × percentage typically denied × average claim amount)
- Clean claim improvement (reduction in claims requiring rework × cost per rework × volume)
Cost Reduction
- Staff efficiency (reduction in FTEs required × loaded cost per FTE)
- System consolidation (elimination of legacy systems × annual license and support costs)
- Reduced payer communications (reduction in phone inquiries × cost per inquiry)
Cash Flow Improvement
- Days in A/R reduction (reduction in days × annual revenue ÷ 365 × cost of capital)
Strategic Value
- Value-based contract performance improvement (increase in quality metric achievement × incentive payment per metric)
- Patient retention (reduction in insurance-related patient dissatisfaction × patient lifetime value × estimated retention improvement)
A rigorous ROI model should also account for implementation costs (software licenses, implementation services, integration development, internal resources), ongoing operational costs (license fees, support costs, maintenance), and should extend across a multi-year period to account for increasing benefits as the organization optimizes the platform over time.
Future Scope: AI and Automation in Insurance Coordination
The convergence of AI, automation, and healthcare insurance coordination represents perhaps the most exciting frontier in health technology. Health Cloud’s integration with Salesforce Einstein and the broader Salesforce platform positions organizations to leverage these capabilities as they mature.
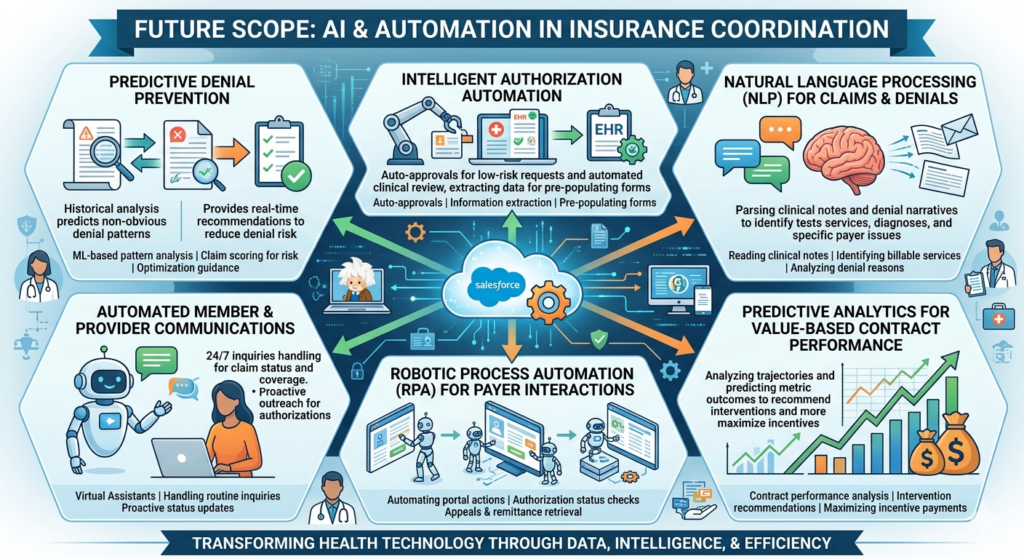
Predictive Denial Prevention
Current denial prevention focuses on rules-based checking: Does this service require authorization? Does the diagnosis support medical necessity for this procedure? Future AI capabilities will leverage machine learning across vast datasets to identify subtle patterns that predict denials.
Einstein can analyze millions of historical claims to identify non-obvious denial predictors: specific combinations of procedure codes, modifiers, and patient characteristics that consistently result in denials from particular payers. Before submission, claims can be scored for risk, with high-risk claims flagged for human review and enhancement.
More ambitiously, AI can recommend specific interventions: “Claims for this procedure with diagnosis X have an 85% denial rate from this payer, but adding diagnosis Y when clinically appropriate reduces denial risk to 12%.” This guidance helps providers optimize documentation in real-time rather than learning from denials after the fact.
Intelligent Authorization Automation
Prior authorization represents a prime candidate for intelligent automation. Many authorization requests involve straightforward scenarios: established patients receiving standard treatments for clearly documented conditions. AI can auto-approve these low-risk requests based on clinical documentation in the EHR, eliminating the manual submission and review process entirely.
For requests requiring clinical review, AI can extract relevant information from clinical documentation, pre-populate authorization forms, and even generate supporting narratives explaining medical necessity based on evidence-based guidelines. This dramatically reduces the burden on clinical staff while improving authorization approval rates through more compelling presentations.
As payer systems become more sophisticated (and as standards like FHIR enable better interoperability), we’ll move toward real-time authorization adjudication at the point of service for an increasing percentage of requests.
Natural Language Processing for Claims and Denials
Clinical documentation contains rich information that’s often difficult to extract and structure for billing purposes. Natural language processing (NLP) can read clinical notes, identify billable services and supporting diagnoses, suggest appropriate codes, and flag documentation gaps that could lead to denials.
Similarly, denial reason narratives (beyond just adjustment reason codes) can be parsed using NLP to identify the specific issues payers have with claims. This structured information can feed both immediate appeal preparation and longer-term process improvement initiatives.
Automated Member and Provider Communications
Chatbots and virtual assistants can handle a significant portion of routine inquiries from members and providers about claim status, coverage details, and authorization status. By accessing Health Cloud’s comprehensive data, these AI assistants can provide accurate, personalized responses without human intervention.
More sophisticated implementations can proactively reach out to members and providers: “Your prior authorization for the procedure scheduled on [date] is still pending. Would you like us to expedite review or reschedule the procedure?” This proactive communication prevents problems before they occur and improves experiences for all stakeholders.
Robotic Process Automation for Payer Interactions
Despite industry progress on electronic transactions, many payer interactions still require manual portal logins, navigation through multiple screens, and data re-entry. Robotic process automation (RPA) can automate these interactions, logging into payer portals to check authorization status, submit appeals, or retrieve remittance information.
Health Cloud can orchestrate these RPA bots, triggering them when specific conditions are met and ingesting the information they retrieve back into member and claim records. This dramatically reduces the manual effort required to interact with payers that haven’t yet fully embraced electronic transactions.
Blockchain for Claims and Authorization Verification
Looking further into the future, blockchain technology could transform claims and authorization verification. A distributed ledger shared between payers and providers could provide immutable, real-time verification of authorizations, eligibility, and claim status without requiring each party to maintain separate systems of record.
While significant standardization and industry cooperation would be required, the potential benefits are substantial: elimination of eligibility verification delays, instant authorization verification, and dramatic reduction in claim status inquiries and payment reconciliation issues.
Predictive Analytics for Value-Based Contract Performance
AI-powered analytics can identify at-risk contract performance early enough to intervene effectively. By analyzing current performance trajectories, patient panel characteristics, seasonal patterns, and external factors, the system can predict: “Based on current trends, you’re projected to miss Quality Metric X by 3 percentage points at year-end, putting $450K of incentive payments at risk.”
More importantly, the system can recommend specific interventions: “Closing care gaps for these 127 patients would improve the metric to threshold. Here are the highest-impact opportunities ranked by patient contactability and intervention complexity.”
Augmented Intelligence for Complex Cases
For complex denials, appeals, or authorization requests requiring expert judgment, AI won’t replace human intelligence but will augment it. The system can surface relevant previous cases, summarize clinical documentation, identify applicable coverage policies, and suggest argumentation approaches—essentially serving as an expert assistant that makes experienced staff more productive and less experienced staff more effective.
This augmented intelligence approach represents the most realistic near-term future for AI in healthcare: not replacing human decision-making but providing better information, context, and recommendations to humans who make final decisions.
Conclusion
Insurance coordination and claims management represent significant operational and financial challenges for healthcare organizations and payers. Fragmented systems, manual processes, adversarial payer-provider dynamics, and increasing complexity from value-based payment models create inefficiency, revenue leakage, and stakeholder frustration.
Salesforce Health Cloud offers a fundamentally different approach: a unified platform that brings together insurance workflows, relationship management, and advanced analytics in a single ecosystem. By providing 360-degree visibility into members and providers, enabling collaborative workflows across organizational boundaries, leveraging AI for predictive insights, and automating routine transactions, Health Cloud transforms insurance coordination from a cost center managing administrative burden to a strategic capability creating competitive advantage.
The real-world results speak clearly. Organizations implementing Health Cloud for insurance coordination consistently achieve:
- Denial rate reductions of 30-50%
- Authorization processing time improvements of 40-60%
- Staff efficiency gains enabling 20-40% productivity improvement
- Days in accounts receivable reductions of 10-20 days
- ROI within 3-12 months with benefits continuing to compound over time
Beyond these quantifiable improvements, Health Cloud enables strategic capabilities increasingly essential for healthcare success: sophisticated value-based contract management, predictive analytics for denial prevention, collaborative payer-provider relationships, and seamless member experiences.
As the healthcare industry continues its digital transformation journey, the organizations that will thrive are those that view operational processes like insurance coordination not as necessary evils but as opportunities for differentiation. When you can verify coverage instantly, secure authorizations efficiently, submit claims cleanly, resolve denials systematically, and provide transparency to all stakeholders, you create better experiences, better financial performance, and better positioning for the value-based future.
At RizeX Labs, we’ve guided dozens of healthcare organizations through this transformation. We’ve seen firsthand how the right technology foundation, thoughtfully implemented with attention to workflows and change management, can revolutionize operations that have frustrated staff and drained resources for decades.
If your organization struggles with insurance coordination inefficiencies, mounting denial rates, prior authorization bottlenecks, or the complexity of value-based contracts, Health Cloud deserves serious consideration. The platform has matured significantly, the implementation methodology has been proven across diverse organizations, and the ROI case has been validated repeatedly.
The question isn’t whether technology can solve these problems—it’s whether your organization is ready to embrace the process change, data discipline, and strategic thinking required to realize technology’s potential. For organizations ready to make that commitment, Health Cloud provides the foundation to transform insurance coordination from an operational headache into a strategic asset.
About RizeX Labs
At RizeX Labs, we specialize in delivering industry-focused Salesforce solutions, including Salesforce Health Cloud for insurance providers and claims coordination. Our expertise combines deep healthcare knowledge with real-world implementation experience to help organizations streamline claims workflows, improve member engagement, and enhance operational efficiency.
We help insurers move beyond fragmented systems—transforming disconnected processes into unified, intelligent workflows that support end-to-end claims lifecycle management beyond hospital environments.
Internal Links:
- Salesforce Admin & Development Training
- Remote Patient Monitoring (RPM) in Salesforce Health Cloud: Transforming Connected Healthcare Delivery
- How to Use AI in Salesforce Health Cloud for Predictive Patient Care (Einstein + Real Use Cases)
- New Releases in Salesforce Health Cloud Spring ’26: What Healthcare Organizations Need to Know
- How to Customize Salesforce Health Cloud Using Lightning Web Components (LWC) for Healthcare Use Cases
- 30 Essential Questions About Salesforce Health Cloud Answered: Beginner to Advanced Guide
- Salesforce Sales Cloud vs Health Cloud: The Strategic CRM Decision That Defines Your Healthcare Business Trajectory
- Using Salesforce Health Cloud for Insurance & Claims Coordination: Beyond the Hospital Walls
External Links:
- Salesforce Official Website
- Salesforce Health Cloud Overview
- Salesforce Revenue Cloud Overview
- Salesforce AppExchange (CLM tools)
- Salesforce CPQ Documentation


